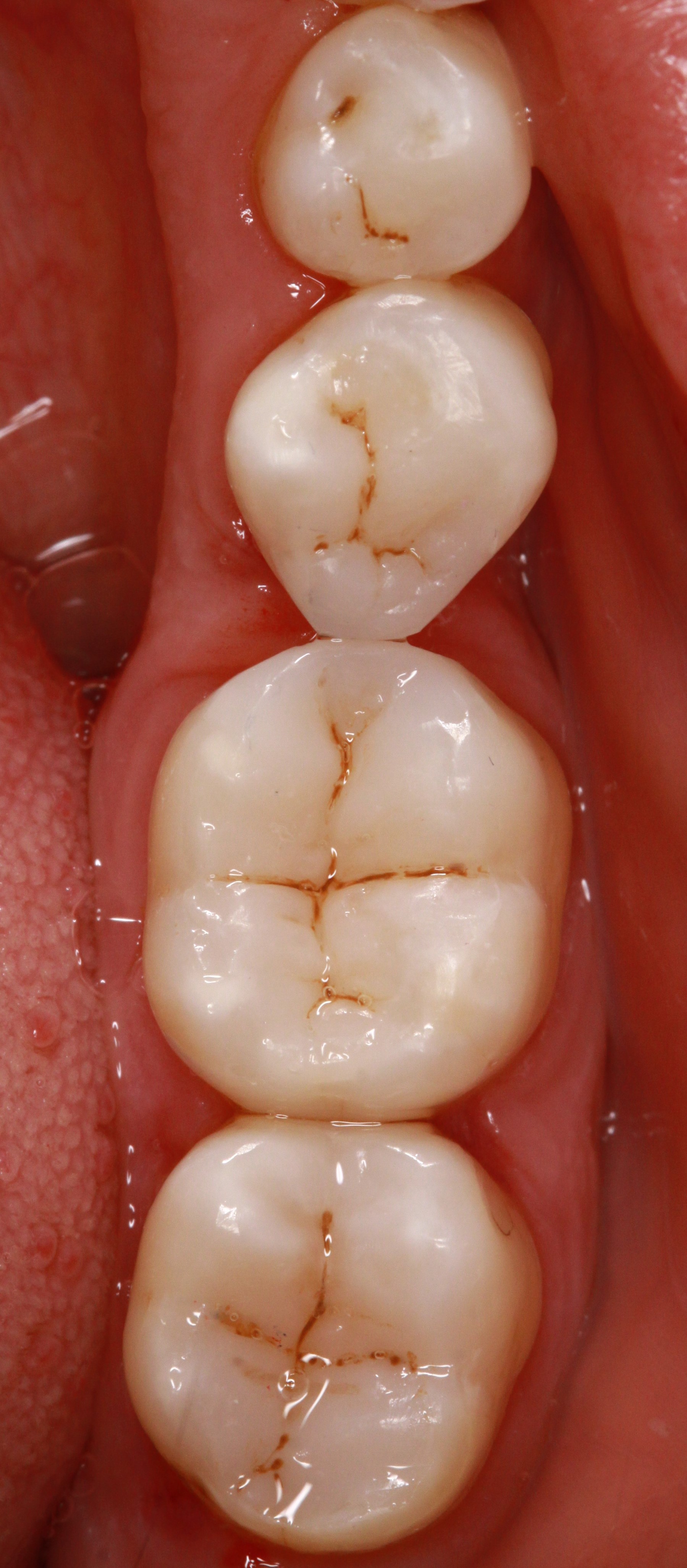
Diamond instruments
Diamond instruments
Diamond instruments are usually rotary and rotationally symmetrical, sometimes oscillating, dental instruments almost always used in drive units (handpieces, contra-angles, turbines) in all areas of dental medicine and technology for widely varying purposes ranging from preparation and trimming conservative or prosthetic restorations to reducing proximal enamel during orthodontic treatment or surgical applications. Certain diamond instruments are for manual use only such as for roughening sites prepared for posts prior to adhering.
Diamond instruments are manufactured by embedding single or multiple layers of multi-surface natural or industrial diamond particles into a layer of bonder (often galvanically bonded or sintered to the metal blank). The edges of the particles abrade tissue and many types of material (mostly hard tooth structure such as enamel and dentine). Worn edges and particles breaking out of the bonder cause the instruments to become blunt. Sintered diamonds and silicone ("rubber") polishers are not only "coated" on the surface, the entire instrument is impregnated with diamond particles making them self-sharpening (but their original size and shape wear down). Colour-coded rings are used for classifying diamond instruments according to their abrasivity (depending on the particle size) ranging from extra-coarse (approx. 150 µm for reducing structure rapidly) to ultra-fine (approx. 15 µm for final finishing).
 Diamond bur
Diamond bur
When manufactured carefully (precise dimensioning of the instrument geometry, quality, sharpness/homogeneity of the particles, steel quality) diamond instruments run smoothly, perform efficiently and are long lasting.
The different shapes and sizes of diamond instruments can be designated numerically and uniformly acc. to DIN EN ISO 6360-1 (e.g. shank length/material, grit size, diameter of the working section).
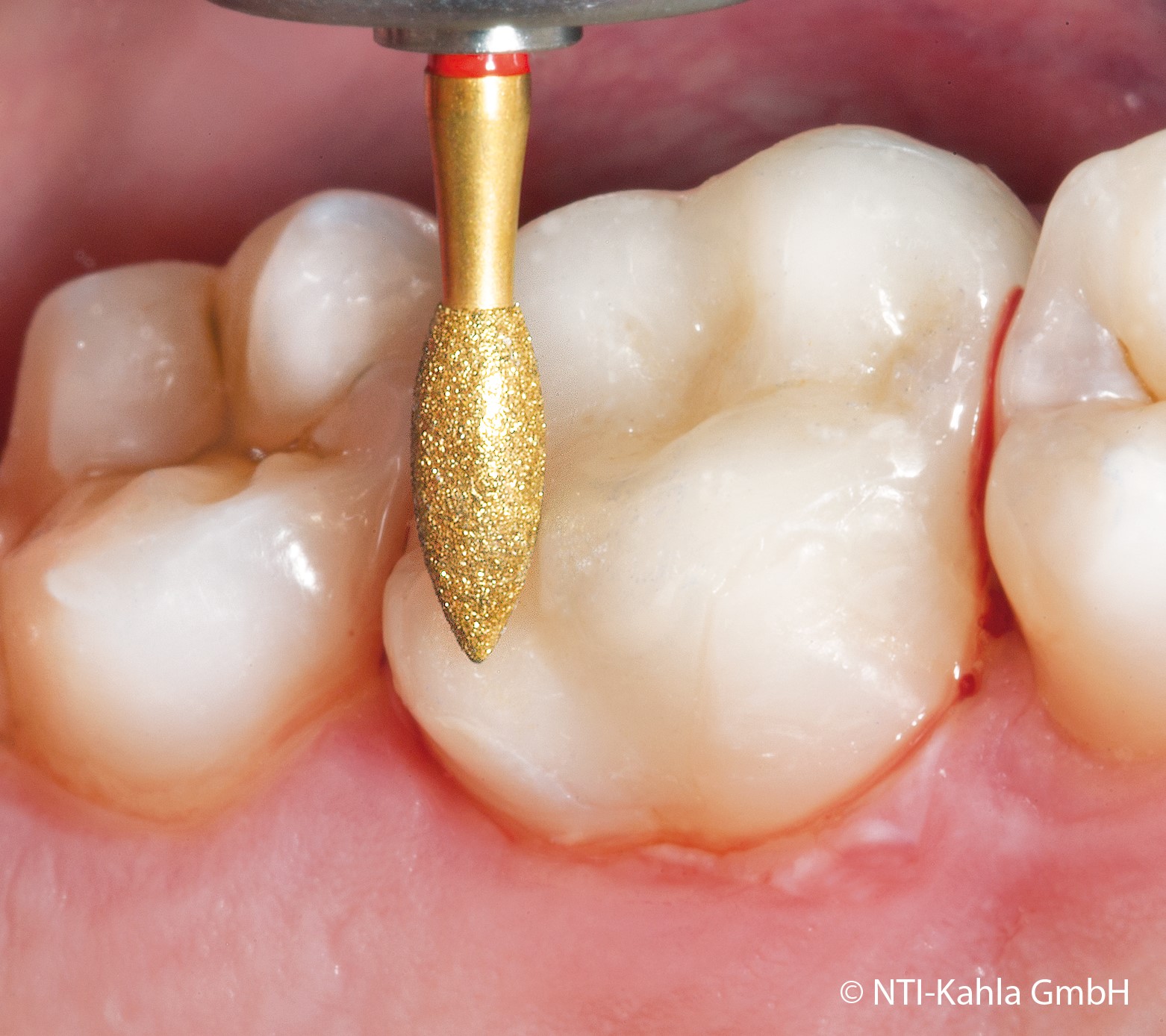 Bud-shaped diamond bur
Bud-shaped diamond bur
Different degrees of frictional force are generated depending on the pressure exerted, speed, diameter, grit size and traction of the drive unit. To prevent the undesirable effects of frictional heat in tissue (e.g. coagulation of proteins) or materials (e.g. cracked zirconia or melted acrylic), diamond instruments are often (a "must" when used intraorally) cooled continually with water. This ensures that dust particles can be flushed away simultaneously thus preventing the instrument clogging. Non-coated grooves, axial or spiralling around the instrument, have the same effect.
The integration of tungsten carbide blades, guide lugs, non-coated areas etc. allows certain structures to be protected against reduction or reduced even more.
Most diamond instruments are autoclavable and for multiple usage. Sterile, disposable diamond instruments are increasingly in use for clinical purposes.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| coronal portion of a natural tooth | Zahnkrone |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

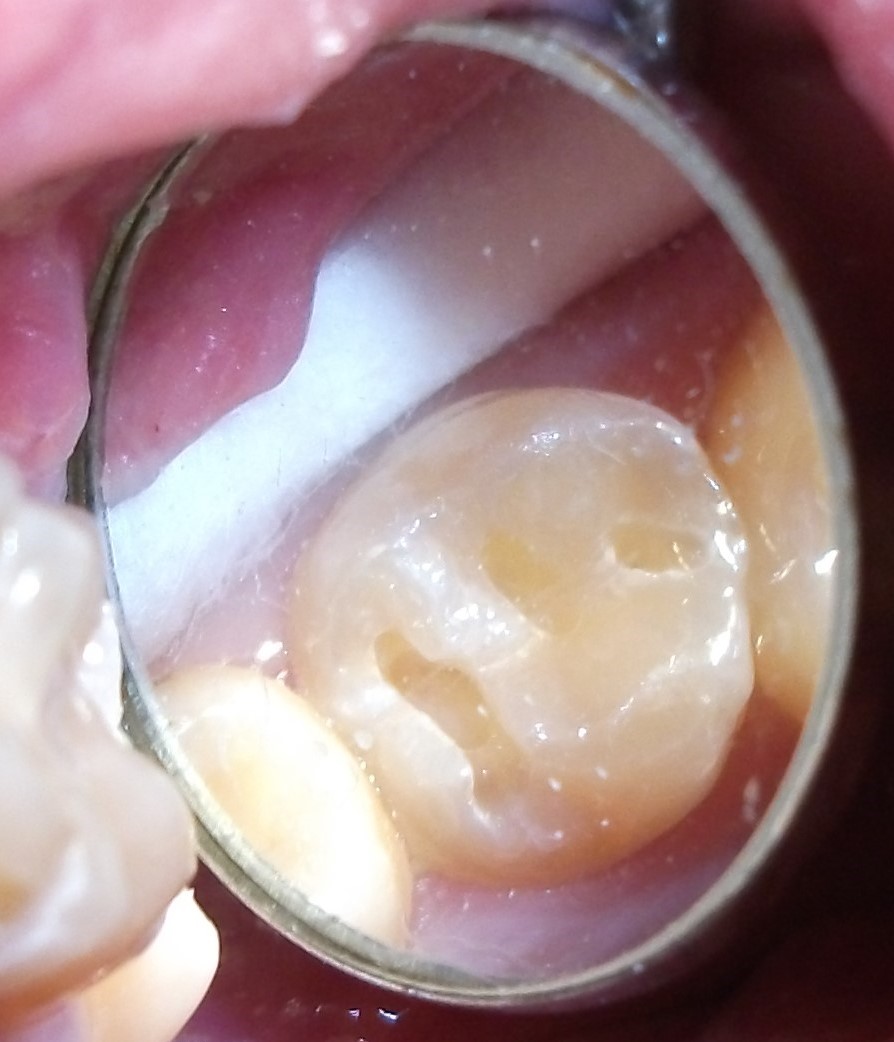 Minimally-invasive preparation and
Minimally-invasive preparation and 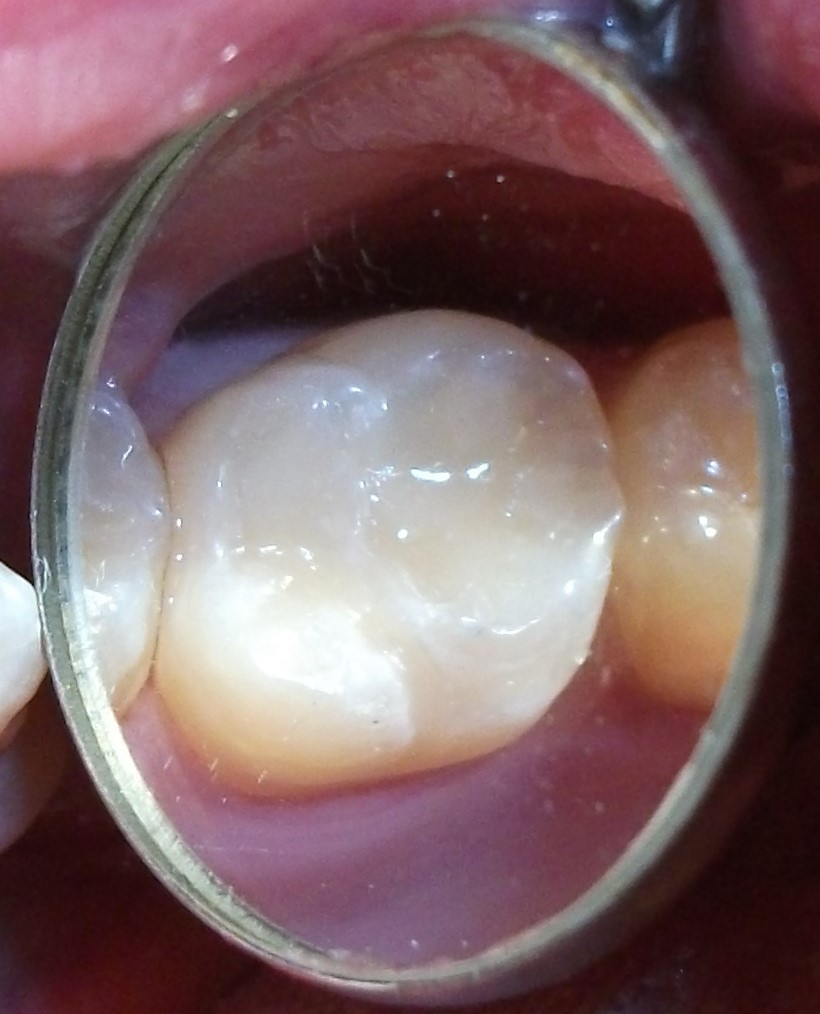 indiscernible composite restoration
indiscernible composite restoration