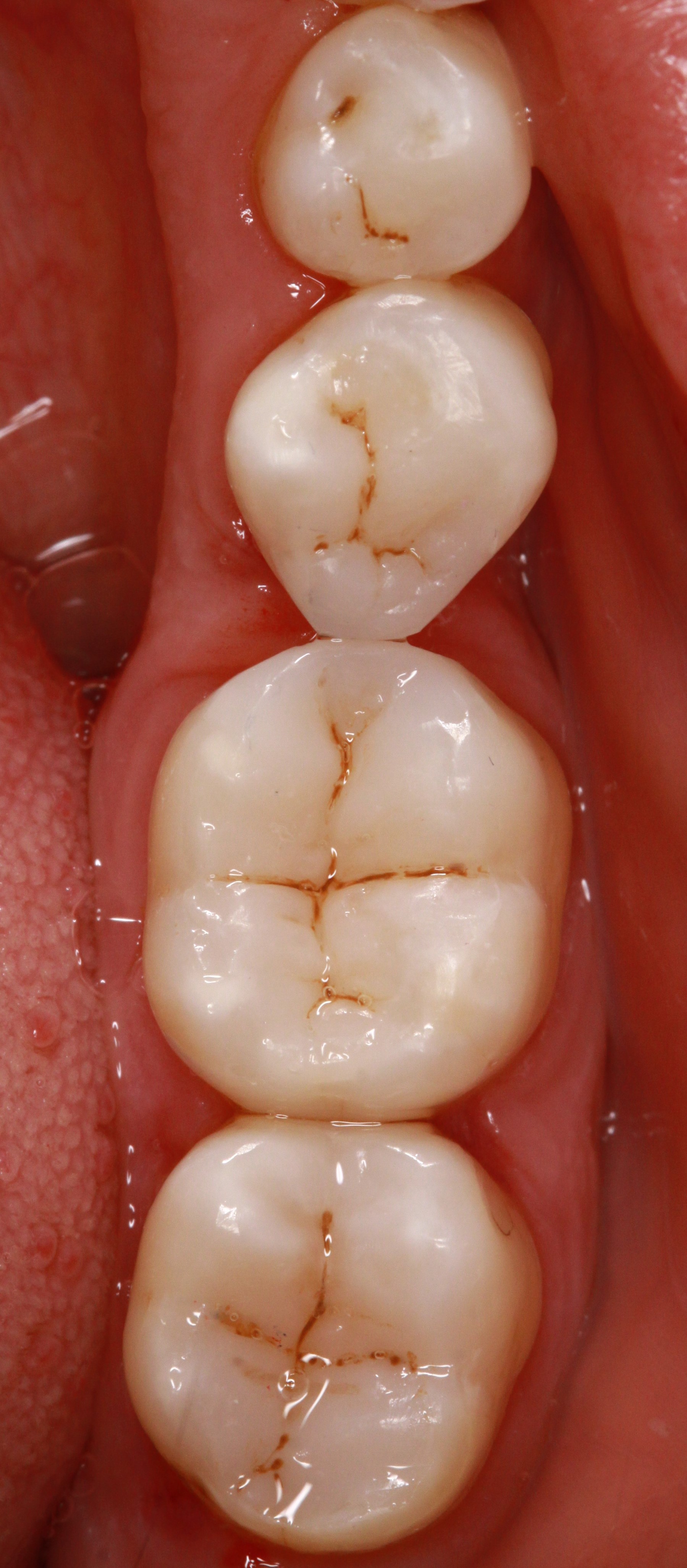
Fixed restorations
Fixed restorations are a part of prosthetics. In particular crowns (though they often do not replace a tooth but only supplement the lost tooth structure of an existing tooth) and bridges as well as bar restorations are described as fixed restorations. Implants replace "fixed" tooth roots in the bone but are not defined as fixed restorations.
In contrast to removable restorations, fixed restorations are rigidly bonded to teeth or implant abutments using adhesive retention or cementation. Restorations, which are fixed for the patient (e.g. by screw-retention or temporary cementation) but are designed to be removable by the dentist, are called "operator-removable". If restorations, which are removable for the patient, are retained on fixed crowns they are called fixed-removable restorations.
A minimum of four periodontally healthy abutments in a favourable alignment (quadrangular) is essential for ensuring stable, statically balanced support per jaw for purely fixed restorations. However, for purely implant-borne fixed restorations in particular, a minimum of six abutments is required in the mandible and even eight abutments in the maxilla due to the lower bone quality. An increase in the number of abutments (e.g. using implants) and also a combination using removable (tissue-borne) restorations can help relieve the natural residual teeth.
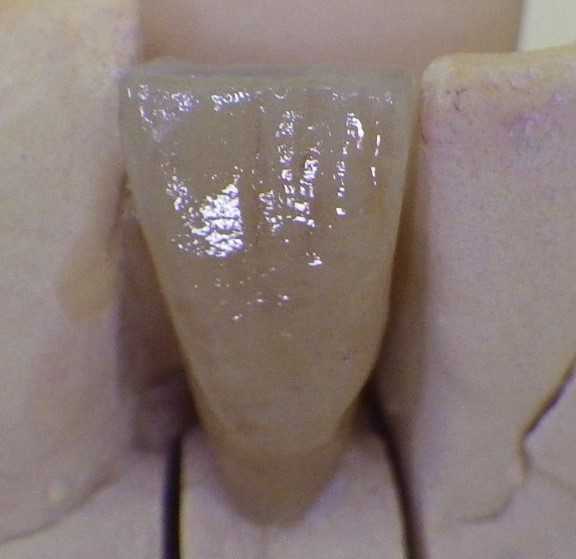 Pontic 42, labial view of single-winged bridge
Pontic 42, labial view of single-winged bridge
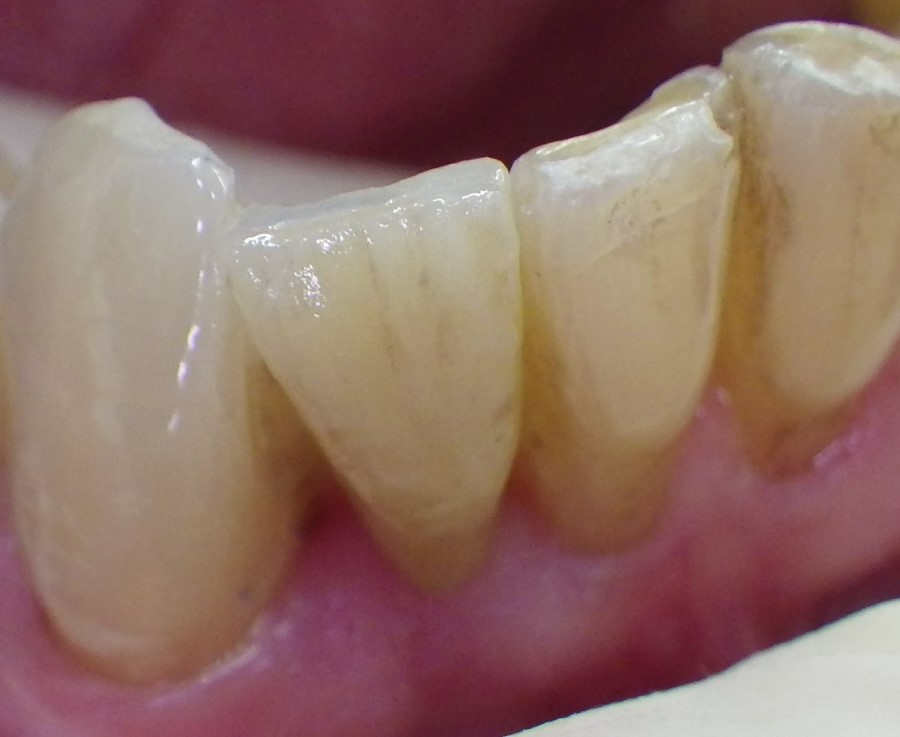 Pontic 42, clinical view of single-winged bridge
Pontic 42, clinical view of single-winged bridge
Features of fixed restorations are periodontal support on abutments, a rigid, immovable connection with the abutment and the subjective sensation of patients of wearing "their own teeth". Care and repair are more difficult compared with removable versions and extending the restoration is generally impossible – especially in the case of (primary) connections with adjacent single crowns for increasing the stability. This is why the previously generally accepted superiority of fixed restorations should be qualified according to each individual case.
A fixed restoration is not only impossible in edentulous cases but also with implants if, as a result of massive bone resorption, the distance between the alveolar ridge level and occlusal plane is too large, which would lead to an excessively forceful leverage effect.
Fixed restorations can be fabricated provisionally (temporary; generally using acrylic and rarely from metal or ceramic), e.g. for testing a new occlusal relationship or for bridging the time required for fabrication of the permanent restoration or other treatment.
Individual components of fixed restorations can be prefabricated (e.g. attachments, other connectors or implant abutments); these can remain unchanged or they can be customised. Final (permanent) fixed restorations are fabricated either from a single material, combinations of materials or by joining different materials using very different procedures, e.g. casting, milling, soldering, welding, grinding, sintering (CAD-CAM), pressing or electroforming.
Temporary luting (short, medium or long-term) can be used for trying in fixed restorations.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

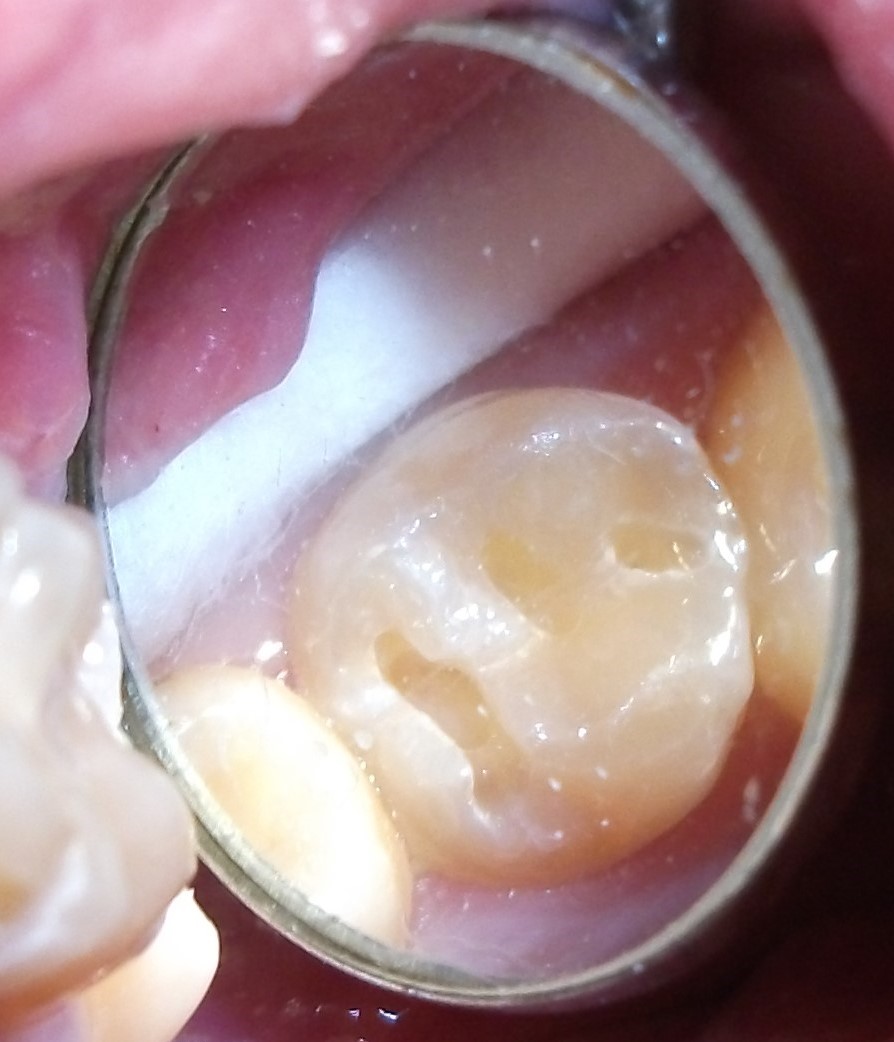 Minimally-invasive preparation and
Minimally-invasive preparation and 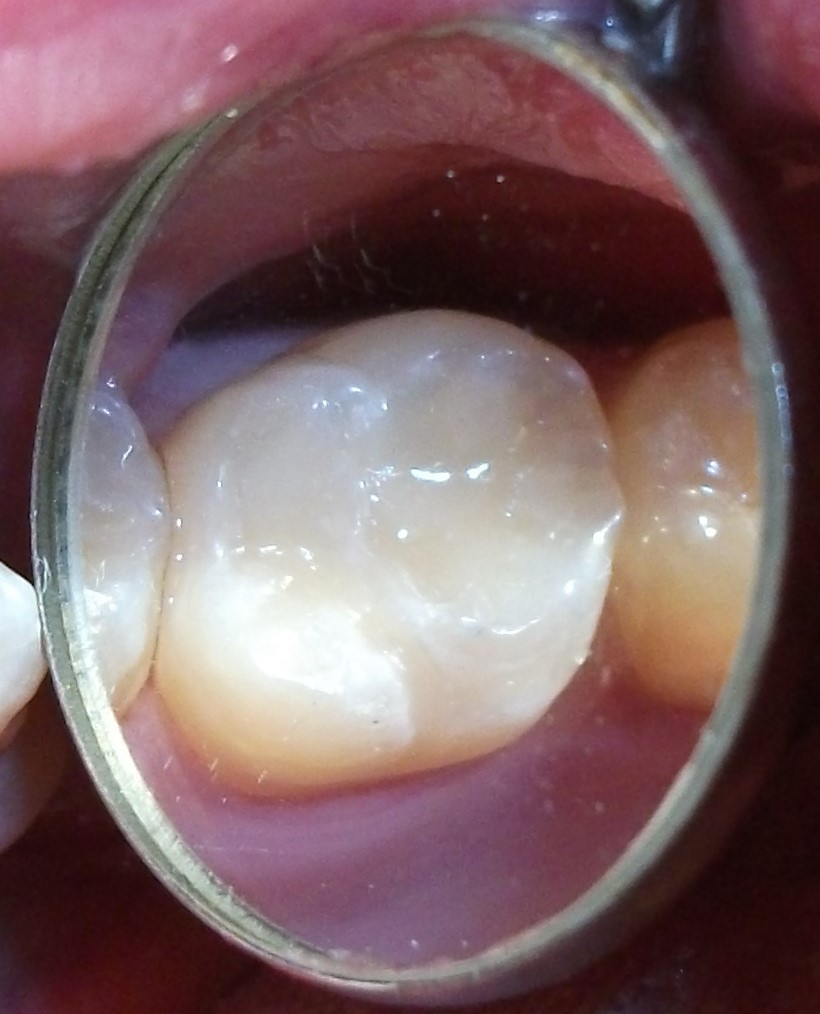 indiscernible composite restoration
indiscernible composite restoration