Double (telescopic) crowns
Double (telescopic) crowns are connectors for retaining fixed/removable appliances. Since they were first fabricated and placed in Germany, they are often referred to as "German crowns".
The removable section can be a coverdenture, partial denture or removable/operator-removable telescopic bridge. As with a slide attachment, telescopic crowns can also be used in cases where sectioned bridgework is required to compensate for non-parallel abutments.
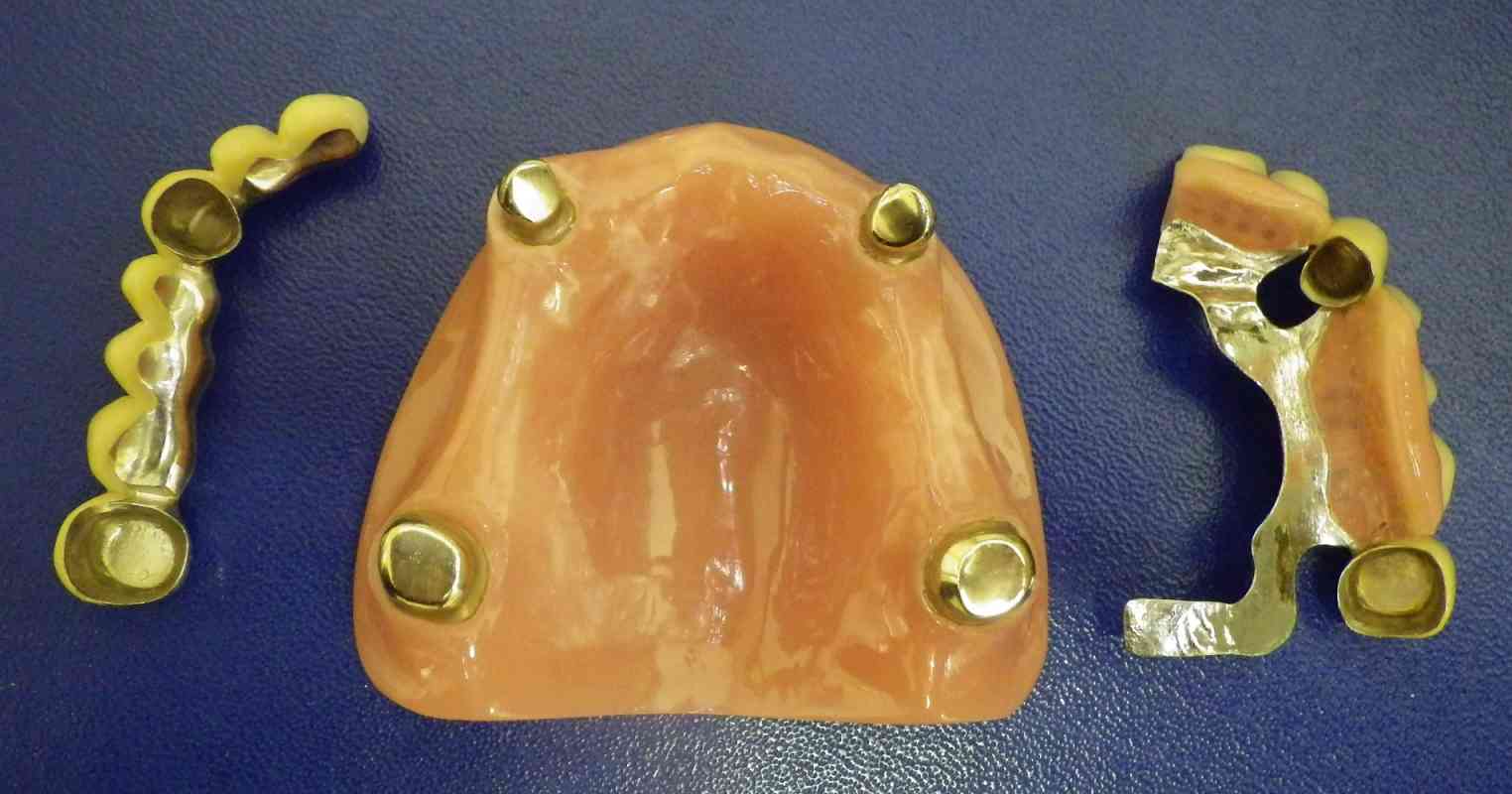 The various types of double crownwork for use in the maxilla
The various types of double crownwork for use in the maxilla
The principle of double crowns involves achieving precision of fit between an outer coping cast into, soldered, welded or adhered to the removable section and a coping screw-retained on an abutment or cemented to a natural abutment, which are congruent in form. Electroformed double crowns require a thin gold outer coping to be electroformed and adhered passively into the denture. Inner copings are usually fabricated singly but may also be splinted ("primary splinting"). The removable section splints the abutments to a certain degree ("secondary splinting") yet abutment teeth bearing telescopic units often exhibit increased physiological mobility.
 4 inner copings milled parallel for a hybrid prosthesis supported on teeth and implants
4 inner copings milled parallel for a hybrid prosthesis supported on teeth and implants
 Two cast inner copings
Two cast inner copings
Whereas classic double crowns were usually cast with the same metal alloy, nowadays combinations of different materials are possible, e.g. metal-free, zirconia inner copings and high-strength plastic outer copings. This rules out metal corrosion (gap corrosion).
If the circumferential walls of the copings are milled/fabricated cylindrically (only possible in theory) in order to achieve "parallel" fit, we speak of "telescopic crowns" and those with tapering walls are known as "conical crowns". A "ring telescope crown" features an outer crown with open occlusal aspect.
After taking a precision impression (digitally or with impression material), a model is cast from it and the inner copings fabricated on the model. The three-dimensional relationship of the copings to each other and the oral structures is recorded with a second ("pick-up" or "fixation") impression. This impression is used for casting the master model and the removable denture section fabricated on it. To avoid non-parallelism, all copings must be in place during cementation.
Normally double crowns are placed on at least 2 abutments per jaw (one per quadrant). The more double crowns are placed, the better the exerted loads are distributed and, should circumstances dictate, the more abutments can be extracted at a later stage without compromising the splinting effect or denture. To achieve at least linear (such as on right and left canines) or, preferably, triangular or four-cornered support (also on distal posterior teeth or implants placed to increase the number of abutments), the abutments must be spread as widely as possible around the arch of the jaw.
The advantages of double crowns include uniform load distribution across the abutments, straightforward handling for the patient, concealed connectors, firm and lasting retention along with the option of involving as many abutments (teeth and implants) as possible. Their drawbacks are the increased effort required for fabrication and higher costs, increased space requirement (loss of tooth structure due to preparation), unpleasant appearance of the inner copings (after removing the denture) and occasionally odours due to colonisation of bacteria in the gap between the copings ("moist chamber").
Double crowns are retained by means of cone-fit, adhesion, sliding friction and suction-retention (capillary effect of the gap). Whereas conical crowns only achieve form fit and full retention after reaching their end position, telescopic crowns do so as soon as the frictive surfaces first touch. If metallic double crowns are not separated for a longer period, are exposed to very heavy loading (bruxism) or if there are burrs or undercuts in the gap between the copings, the metal surfaces of the inner and outer copings may "cold weld" together and/or jam.
After fitting, double crowns usually have to be tried in repeatedly for a few days before they can be placed/removed smoothly. This involves displacing the teeth and trimming microscopically rough areas to eliminate minimal inaccuracies of fit. If dentures with double crowns are not worn for a longer period of time such as during an illness, they may become impossible to place due to, e.g. the teeth drifting so that the abutments are no longer parallel.
In certain types of double crowns the occlusal space between the two copings compensates for mucosal resilience, the denture may sink in to compensate for the material worn off the contacting surfaces of conical copings. Friction lost by double crowns can be restored by retrofitting or activating existing friction units such as friction-fit pins or press-stud attachments. This is the basic principle of special double crown systems such as the non-frictive ("clearance fit") "Marburg double crown".
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| osteoinductive | osteoinduktiv |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

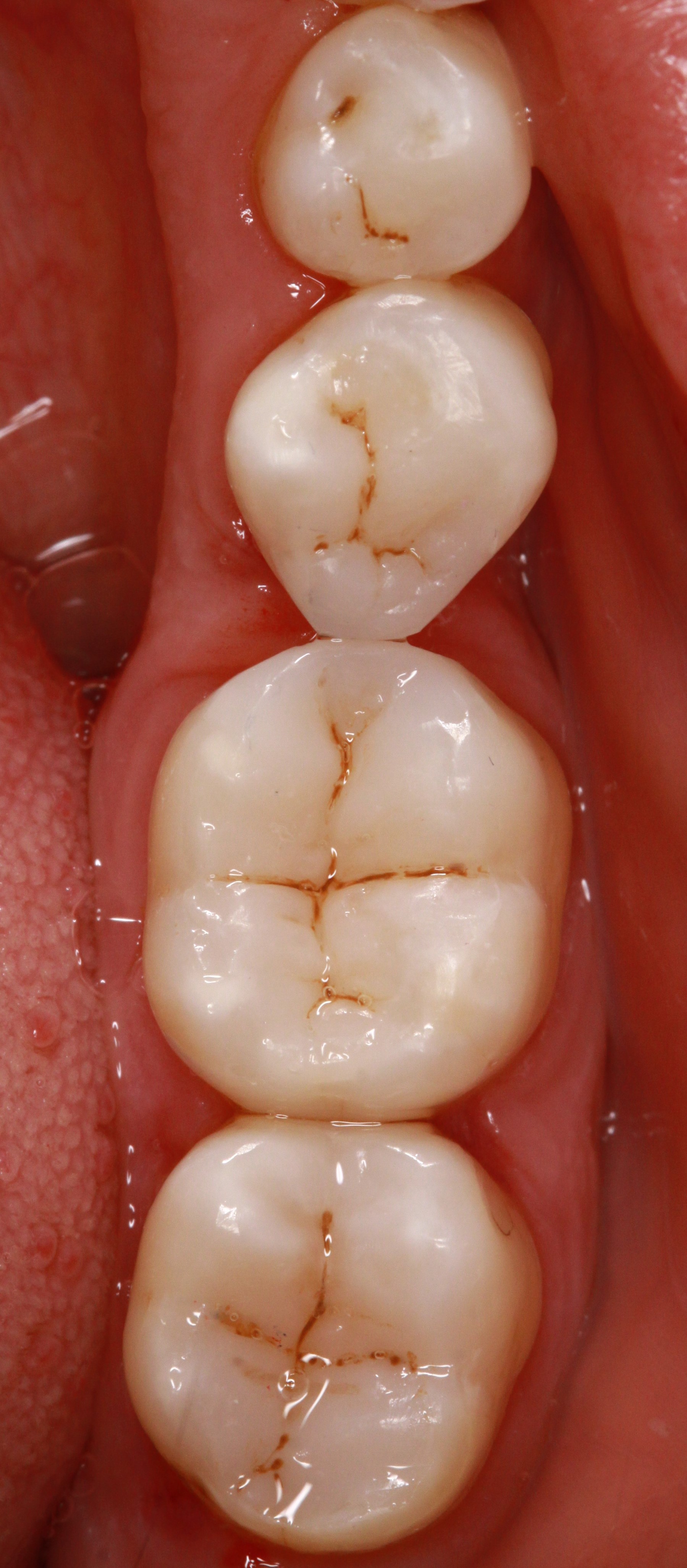
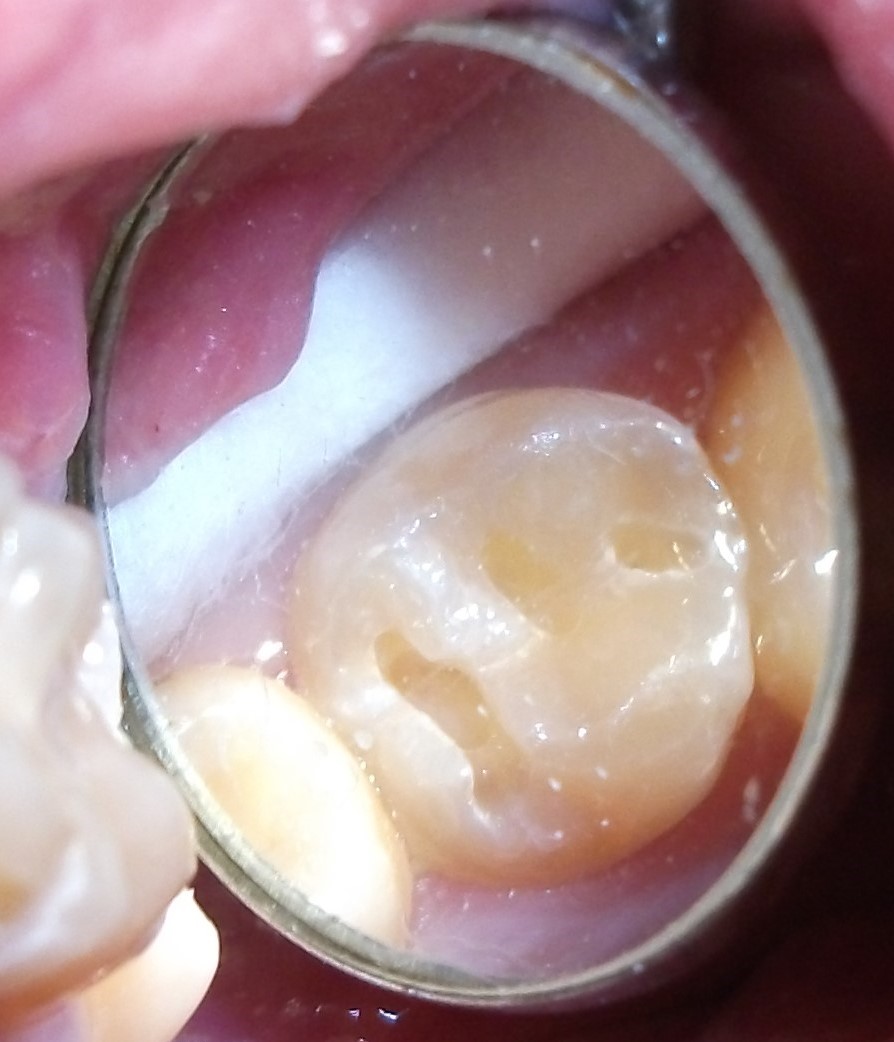 Minimally-invasive preparation and
Minimally-invasive preparation and 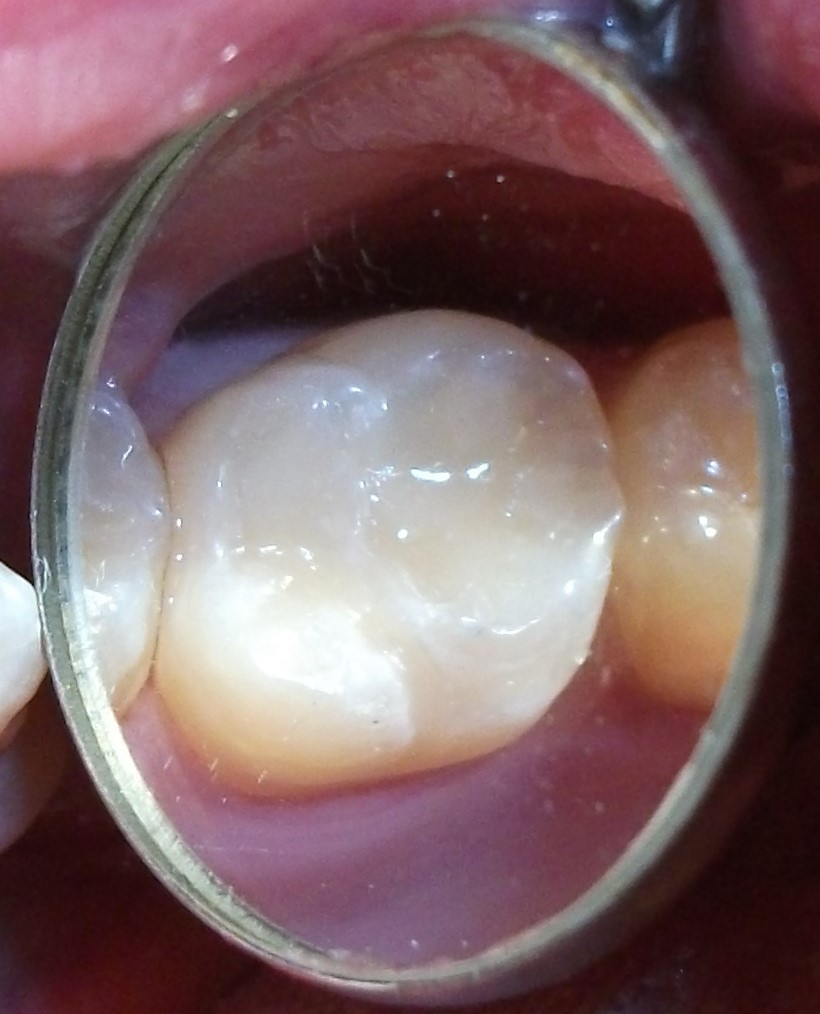 indiscernible composite restoration
indiscernible composite restoration