Bone augmentation
Bone augmentation
Targeted build-up of tissue is referred to as augmentation.
The aim of bone augmentation procedures in dentistry is, on the one hand, the reconstruction of lost bony substance, e.g. in the case of periodontal defects (filling of intrabony pockets) or atrophy of the alveolar ridge and, on the other hand, gaining additional bone volume in areas previously without bone, e.g. in the extraction socket (socket preservation) or at the sinus floor (sinus floor augmentation).
Generally, additional (resorbable or non-resorbable) materials are used for augmentation:
This may involve membranes, which are mainly used for protecting the augmentation area against ingrowing mucosa and connective tissue (guided bone regeneration, GBR). Most granulated bone augmentation materials can be synthetic in origin; animal materials are frequently bovine (i.e. cattle) bone. Natural bone often provides crucial structural benefits compared with synthetic materials, such as very high porosity, which facilitates storage of tissue fluids and penetration of newly formed autogenous bone.
In the case of human bone a differentiation is made between autografting (donor is recipient), involving removal of bone from other regions of the jaw or body, and allografting (donor ≠ recipient), i.e. from cadaver bone.
Any foreign tissue must be very thoroughly cleaned of viable tissue (sterilisation, denaturation of proteins, removal of organic components etc.) to exclude the risk of infection.
Some augmentation procedures require a second intervention in a different region and/or at a different time, e.g. to harvest graft material or remove non-resorbable materials or auxiliary devices.
Bone augmentation procedures are often used to prepare for or accompany implant placement to achieve an aesthetic and functionally optimal implant position. In addition to distraction osteogenesis, the gold standard is augmentation using autologous bone in the form of collected bone chips mixed with autologous blood; recently also using bone cells cultivated in a tissue culture (bone tissue engineering), above all in the form of an autologous block graft.
Bone blocks extracted from other regions are secured in position at the required implant site using membranes, pins, screws etc. Typical areas for bone augmentation in the form of an onlay graft are the posterior region of the mandible (compensation of alveolar ridge atrophy) and the anterior region of the maxilla (reinforcing the labial bone lamella).
The anticipated loss of volume of the graft of up to 50% during the healing phase can be compensated for by initially increasing the size of the graft.
While autologous bone heals completely, osteoconductive or osteoinductive foreign materials can often be resorbed only partially and very slowly and remain detectable even after many years.
The success of augmentation can be promoted by the use of growth factors (mainly proteins, hormones), which stimulate bone growth (e.g. BMPs = bone morphogenetic proteins).
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| speed | Drehzahl, Empfindlichkeit, Empfindlichkeitsklasse, Tourenzahl, Umdrehungszahl, Umdrehungen, Rotationsgeschwindigkeit |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

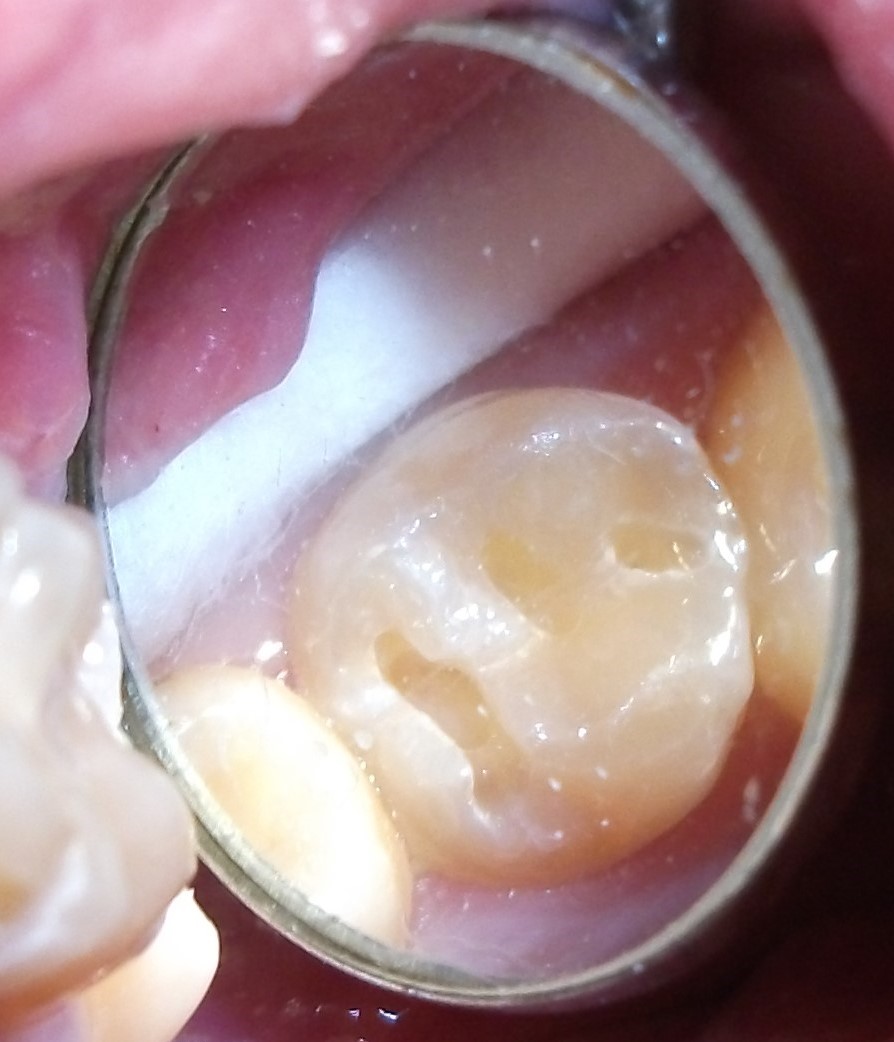 Minimally-invasive preparation and
Minimally-invasive preparation and 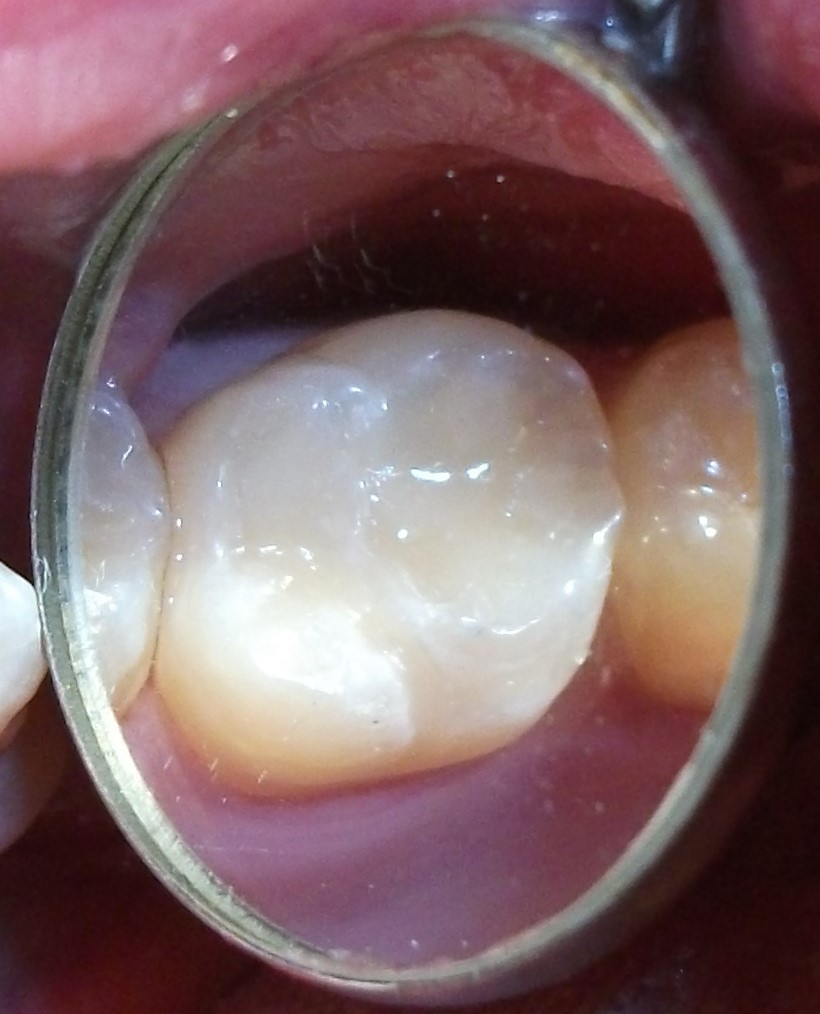 indiscernible composite restoration
indiscernible composite restoration