Membranes
Membranes have been used in dental medicine since about 1980 for covering naturally existing, pathologically caused or synthetically created areas of tissue. They function as a barrier. They are intended forpreventing the growth of unwanted tissue into the boundary area as well as shielding and promoting the formation of tissue required within the area using GTR/GBR. The ideal membrane should have the following characteristics: not trigger immune response, non-toxic (biocompatibility), no risk of infection, formable, adaptable and trimmable, adequately firm/rigid and positionally stable, if necessary permeable for substances yet impermeable to cells, time-determinable spacer function, predictable biological degeneration where required.
Non-resorbable membranes
Non-resorbable membranes can, for example consist of cellulose ester, PTFE or titanium. A second surgical intervention is always required to remove them.
Cellulose ester membranes
The first generation of membranes used (approx. 1980) for shielding against bacteria.
PTFE membranes
Flexible, tear-resistant membranes made from ePTFE (expanded polytetrafluorethylene =Teflon®) with micropores, which make exposure a low risk as no cells or microorganisms can pass through. Sometimes they are reinforced with titanium mesh, making them firm and dimensionally stable; highly suitable for covering extensive augmented areas.
Titanium membranes
These approx. 30 µm thick titanium foils are highly suitable for GBR and alveolar ridge augmentation. They are completely impervious and can be prestressed.
Resorbable membranes
No second intervention is required for removing resorbable membranes due to their integration in the tissue. They are the preferred choice where anticipated that permanent full coverage of the membrane by tissue will be possible and tissue support is not the main priority.
The only resorbable membranes used in the dental sector consist of alloplastic materials. In dentistry we differentiate between hydrophobic, synthetic polymer membranes (e.g. made from polylactide) and hydrophilic, xenogeneic (e.g. bovine or porcine) collagen membranes.
Polylactide membranes
These mostly multi-layer membranes are initially rigid but formable intraorally and mainly used for GTR in periodontology and less commonly for GBR. They comprise polymers of the two enantiomers (D and L form) of lactic acids, if necessary supplemented by portions of glycolide. After a 20-week period in situ these membranes begin to degrade hydrolytically over intermediate stages into the end products water and CO2. This process is complete after approx. one year.
Collagen membranes
These membranes are of animal origin (mostly cattle or pigs) and require careful pretreatment in order to prevent the transfer of pathogens. The collagen structure is differentiated between more rigid (synthetic), cross-linked materials and more flexible (native, natural), non-cross-linked materials. Indications for collagens are stabilising extraction alveoli, coverage of bone defects and augmentation materials, prerestorative alveolar ridge augmentation and periodontal surgery.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| heavily stippled | grob genarbt |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

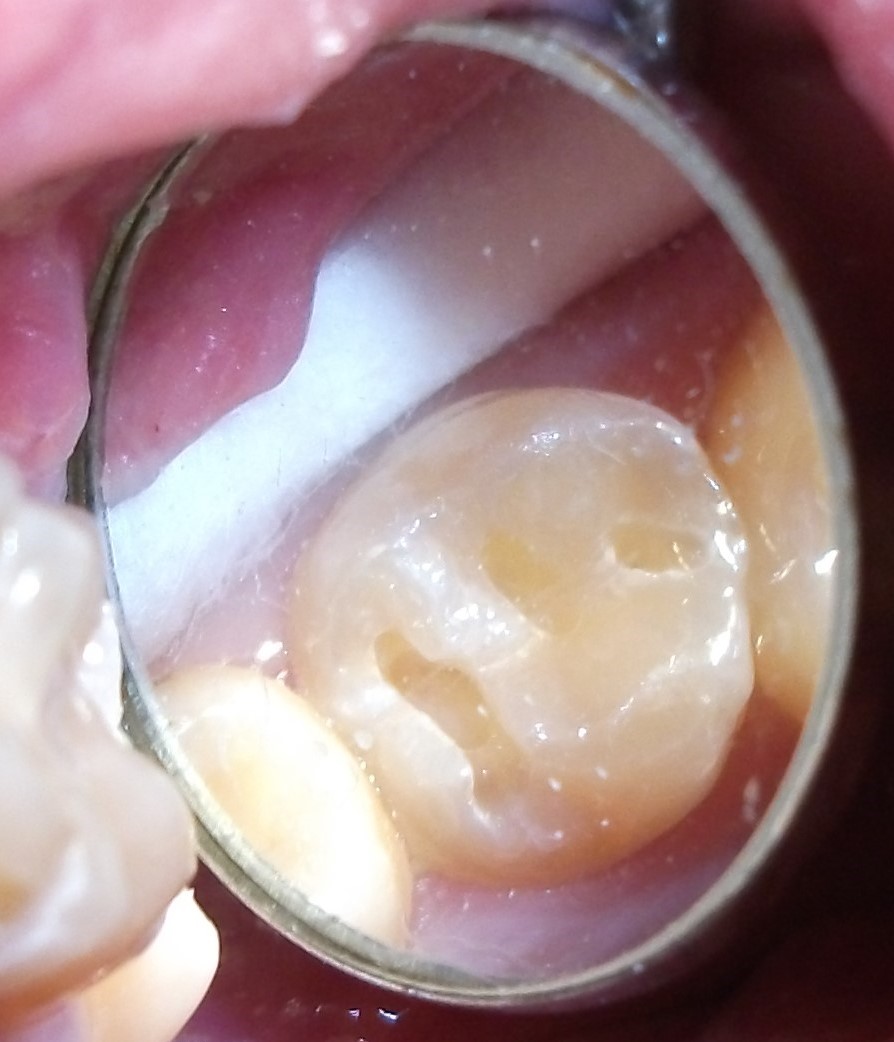 Minimally-invasive preparation and
Minimally-invasive preparation and 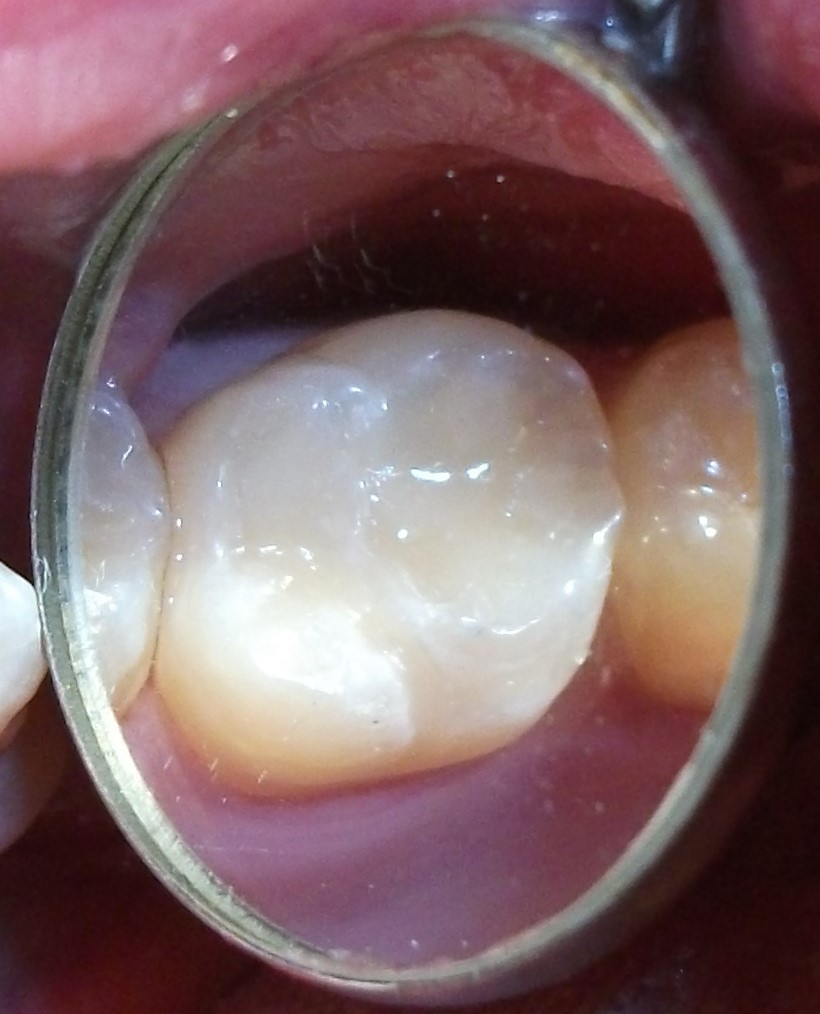 indiscernible composite restoration
indiscernible composite restoration