Membranes
Membranes have been used in dental medicine since about 1980 for covering naturally existing, pathologically caused or synthetically created areas of tissue. They function as a barrier. They are intended forpreventing the growth of unwanted tissue into the boundary area as well as shielding and promoting the formation of tissue required within the area using GTR/GBR. The ideal membrane should have the following characteristics: not trigger immune response, non-toxic (biocompatibility), no risk of infection, formable, adaptable and trimmable, adequately firm/rigid and positionally stable, if necessary permeable for substances yet impermeable to cells, time-determinable spacer function, predictable biological degeneration where required.
Non-resorbable membranes
Non-resorbable membranes can, for example consist of cellulose ester, PTFE or titanium. A second surgical intervention is always required to remove them.
Cellulose ester membranes
The first generation of membranes used (approx. 1980) for shielding against bacteria.
PTFE membranes
Flexible, tear-resistant membranes made from ePTFE (expanded polytetrafluorethylene =Teflon®) with micropores, which make exposure a low risk as no cells or microorganisms can pass through. Sometimes they are reinforced with titanium mesh, making them firm and dimensionally stable; highly suitable for covering extensive augmented areas.
Titanium membranes
These approx. 30 µm thick titanium foils are highly suitable for GBR and alveolar ridge augmentation. They are completely impervious and can be prestressed.
Resorbable membranes
No second intervention is required for removing resorbable membranes due to their integration in the tissue. They are the preferred choice where anticipated that permanent full coverage of the membrane by tissue will be possible and tissue support is not the main priority.
The only resorbable membranes used in the dental sector consist of alloplastic materials. In dentistry we differentiate between hydrophobic, synthetic polymer membranes (e.g. made from polylactide) and hydrophilic, xenogeneic (e.g. bovine or porcine) collagen membranes.
Polylactide membranes
These mostly multi-layer membranes are initially rigid but formable intraorally and mainly used for GTR in periodontology and less commonly for GBR. They comprise polymers of the two enantiomers (D and L form) of lactic acids, if necessary supplemented by portions of glycolide. After a 20-week period in situ these membranes begin to degrade hydrolytically over intermediate stages into the end products water and CO2. This process is complete after approx. one year.
Collagen membranes
These membranes are of animal origin (mostly cattle or pigs) and require careful pretreatment in order to prevent the transfer of pathogens. The collagen structure is differentiated between more rigid (synthetic), cross-linked materials and more flexible (native, natural), non-cross-linked materials. Indications for collagens are stabilising extraction alveoli, coverage of bone defects and augmentation materials, prerestorative alveolar ridge augmentation and periodontal surgery.
PROBIEREN SIE ES EINFACH AUS !!!
Von uns erhalten Sie professionelle Unterstützung.
Treten Sie mit uns in Kontakt oder nutzen Sie unser Kontaktformular.
Wort des Tages
| Deutsch | Englisch |
|---|---|
| Kontermutter | locknut |
Schwerpunkttext des Monats
Totalprothesen Totalprothesen
Da bei der TP keine Informationen über Bisshöhe, Bisslage, Zahnstellung, etc. aus noch vorhandenen Zähnen abgeleitet werden können, ist die schrittweise Rekonstruktion von Kieferrelation und Weichteilstützung, Funktion und Ästhetik anhand anatomischer Gegebenheiten eine besondere Herausforderung. Die Konstanz von Messgrößen wie etwa der Ruheschwebelage oder das Ausmaß ihrer Veränderlichkeit durch Zahnverlust und Zahnersatz sind dabei umstritten. Zur Herstellung von TP werden traditionell mit konfektionierten Löffeln Situationsabformungen der Kiefer und ggf. auch alter Prothesen abgenommen. Auf den Situationsmodellen erstellte individuelle Abformlöffel (Funktionslöffel) oder vorhandene Prothesen dienen nach Anpassung und Ergänzung (z.B. mit Thermoplasten, Silikonen) zur Funktionsabformung. Standfestes, langsam härtendes Abformmaterial (z.B. PVS) führt einerseits zu einer je nach Resilienz der Schleimhaut unterschiedlichen Kompression, so dass eine gleichmäßige Druckverteilung resultiert, um späteren Druckstellen vorzubeugen. Außerdem werden die Funktionsbewegungen (Schluck-, Zungen-, Mund-, Kiefer- und Lippenbewegungen) erfasst, um anatomische und funktionelle Grenzen (etwa zu beweglichen Schleimhautanteilen, Bändern oder dem Gaumensegel) freizuhalten. Bei der TP wird so im Oberkiefer eine Saughaftung angestrebt (distale Abschlusskante auf der Grenze zwischen hartem und weichem Gaumen, "A(h)"-Linie), im Unterkiefer zumindest eine ruhige Lage.
Die Bissregistrierung und Festlegung von Mittellinie, Kauebene und Bisshöhe erfolgt anhand von Schablonen mit Bisswällen oder Pfeilwinkelregistrat, die Überprüfung etwa durch Sprechproben. Zur arbiträren Scharnierachsenbestimmung kann eine Gesichtsbogenübertragung dienen. Eine Anprobe der auf Kunststoffschablonen in Wachs aufgestellten konfektionierten Prothesenzähne erlaubt die Überprüfung von Ästhetik, Halt, Okklusion, Artikulation und Sprachfähigkeit vor der Fertigstellung. Sie erfolgt im zahntechnischen Labor, es werden vielfältige Verfahren mit Kalt- und Heißpolymerisaten, Pressen, Stopfen. Spritzen und Gießen, Küvetten oder Vorwällen etc. angewendet. Nach abschließender Einstellung von Okklusion und Artikulation, Ausarbeitung und Politur erfolgt die Eingliederung.
Neuerdings kann dieser seit Jahrzehnten etablierte Ablauf mit fünf bis sechs Sitzungen durch weitgehende Digitalisierung deutlich (auf zwei bis drei Termine) verkürzt werden. Verschiedene Hersteller bieten die Übertragung am Patienten gewonnener Daten in ein computergestütztes virtuelles System an. Mittels CAD-Programmen werden im virtuellen Artikulator digitalisierte Patientenanatomie und konfektionierte Zähne oder Zahnreihen in Beziehung gesetzt, per CAM-Verfahren wird dann die Prothesenbasis aus einem Rohling ausgefräst. Die Zahnreihen sind entweder voraufgestellt im Fräs-Rohling integriert (TP ist sofort fertig) oder werden aus konfektionierten Zähnen aufgestellt (Wachsanprobe und Anpassungen möglich). |

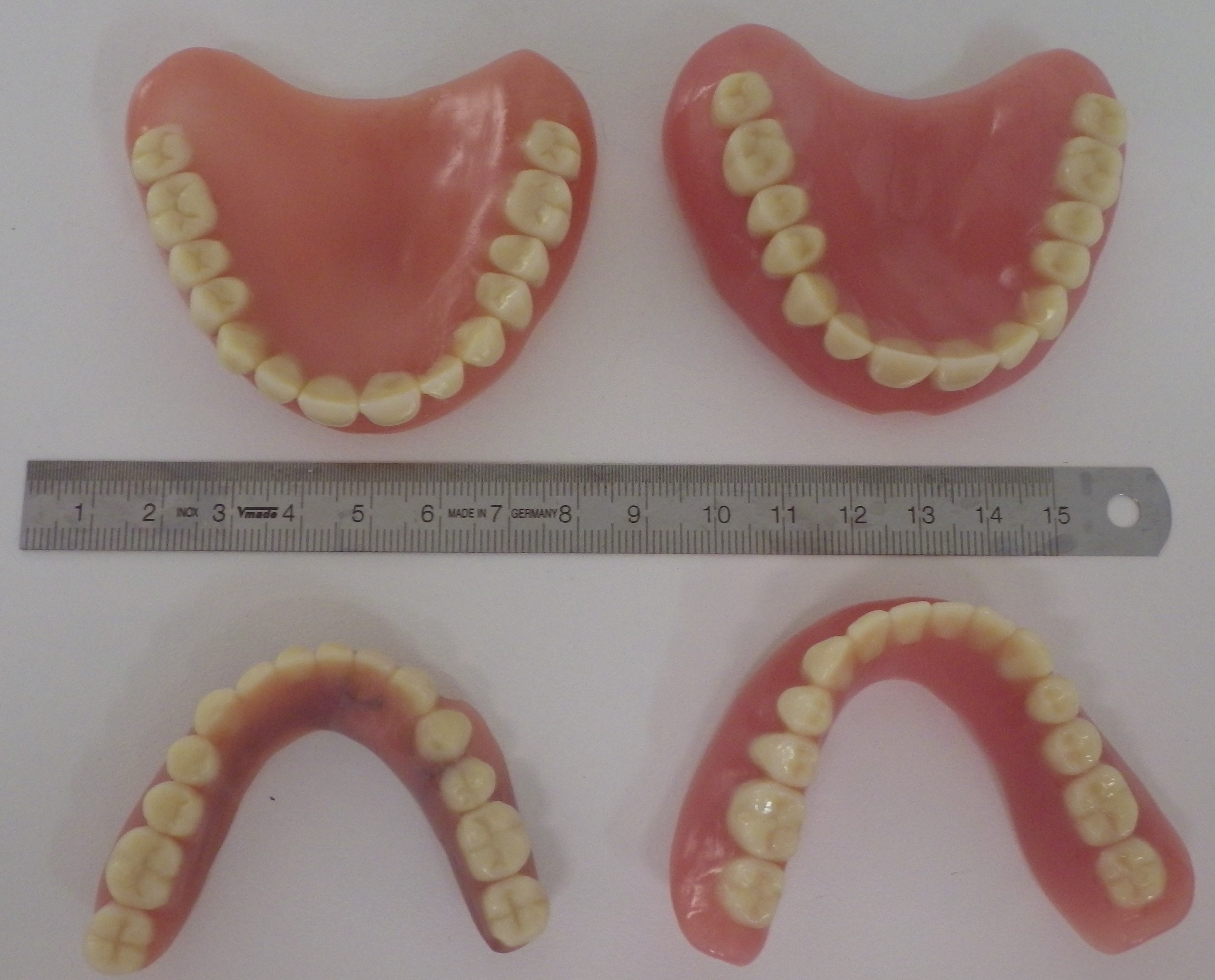 Totalprothesenoberseiten alt/neu
Totalprothesenoberseiten alt/neu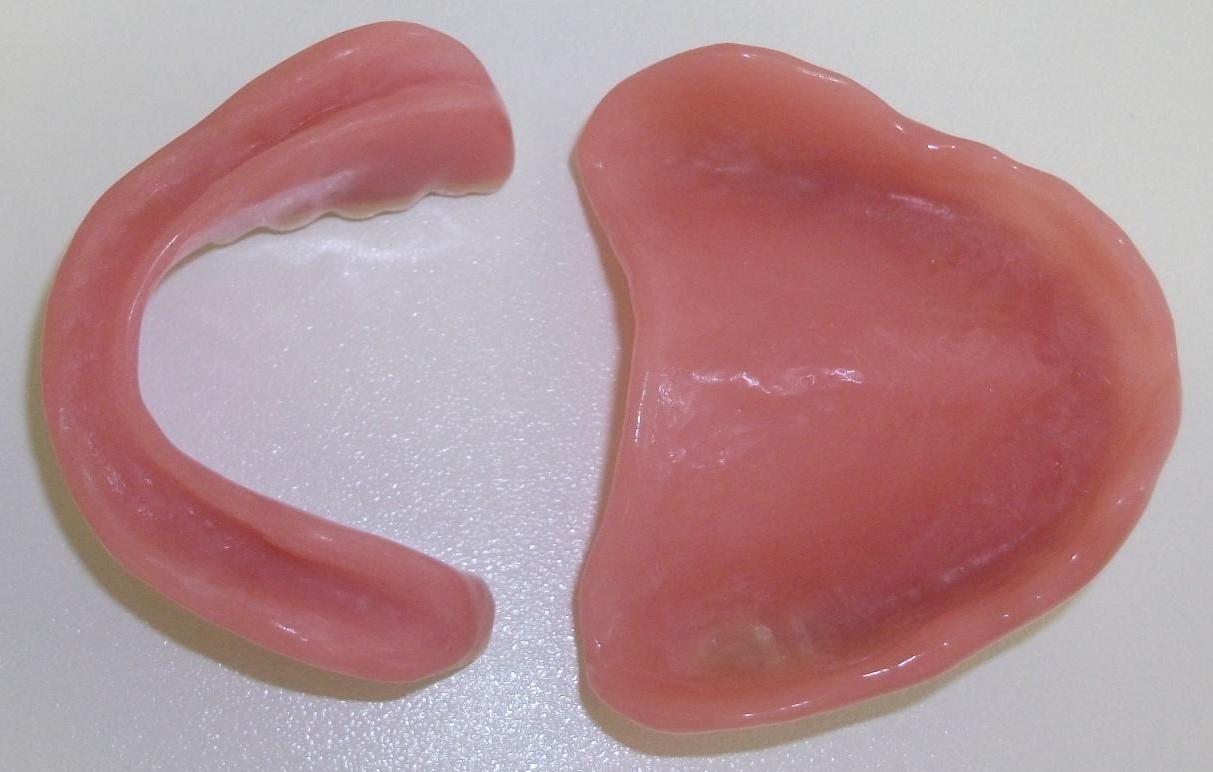 Totale Unterseite
Totale Unterseite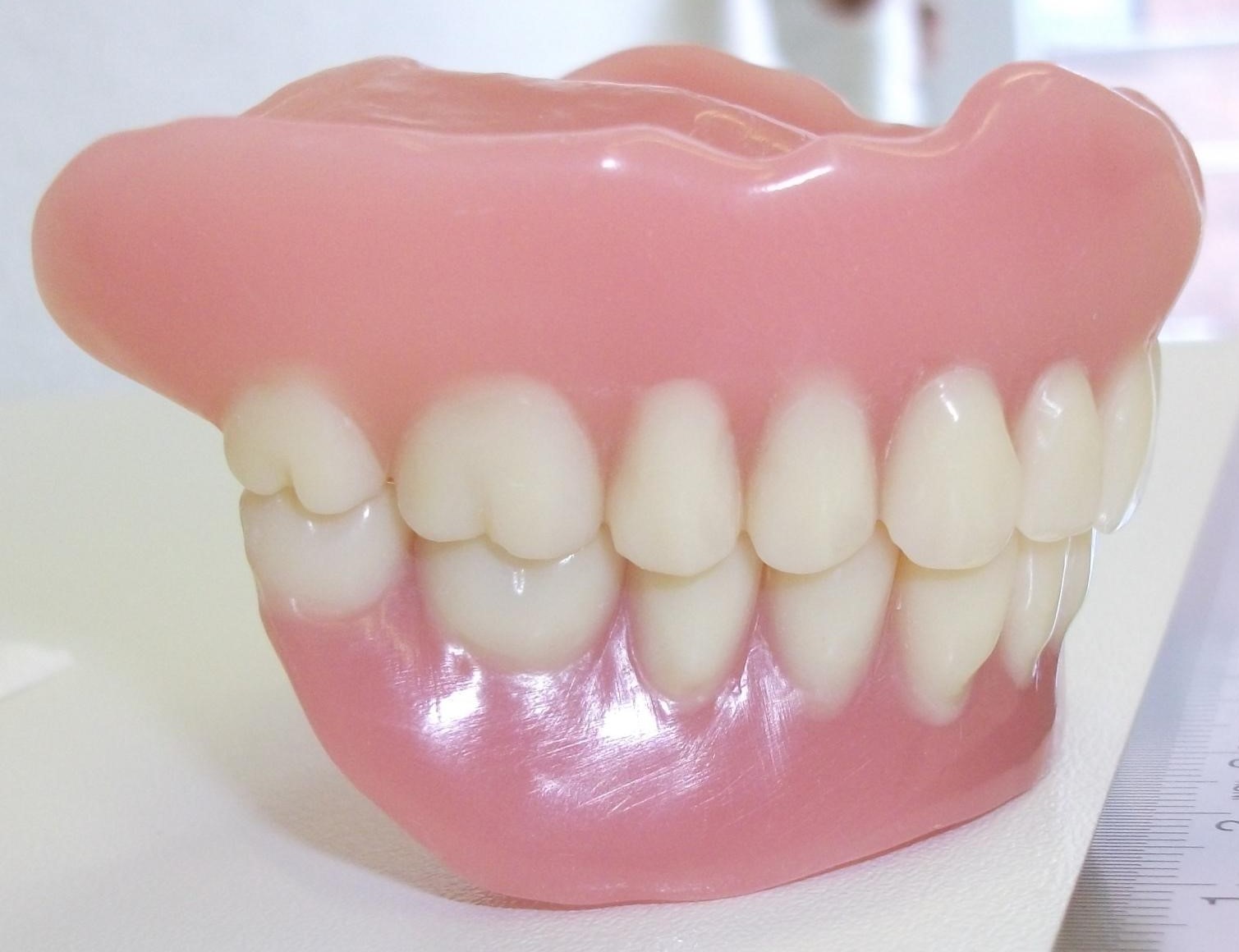 Totale Seitenansicht
Totale Seitenansicht