Fixed/removable prosthetics
Fixed/removable prosthetics
Fixed/removable prosthetic restorations form a part of prosthodontics. Unlike with full dentures, fixed/removable restorations always involve natural teeth and/or implants. As opposed to purely removable dentures (which include full dentures and partials retained on natural teeth with clasps), fixed/removable dentures consist of two sections, i.e. one fixed and one removable section.
 Fixed/removable denture including CoCr, clasps, precision attachment and double crowns (demo model)
Fixed/removable denture including CoCr, clasps, precision attachment and double crowns (demo model)
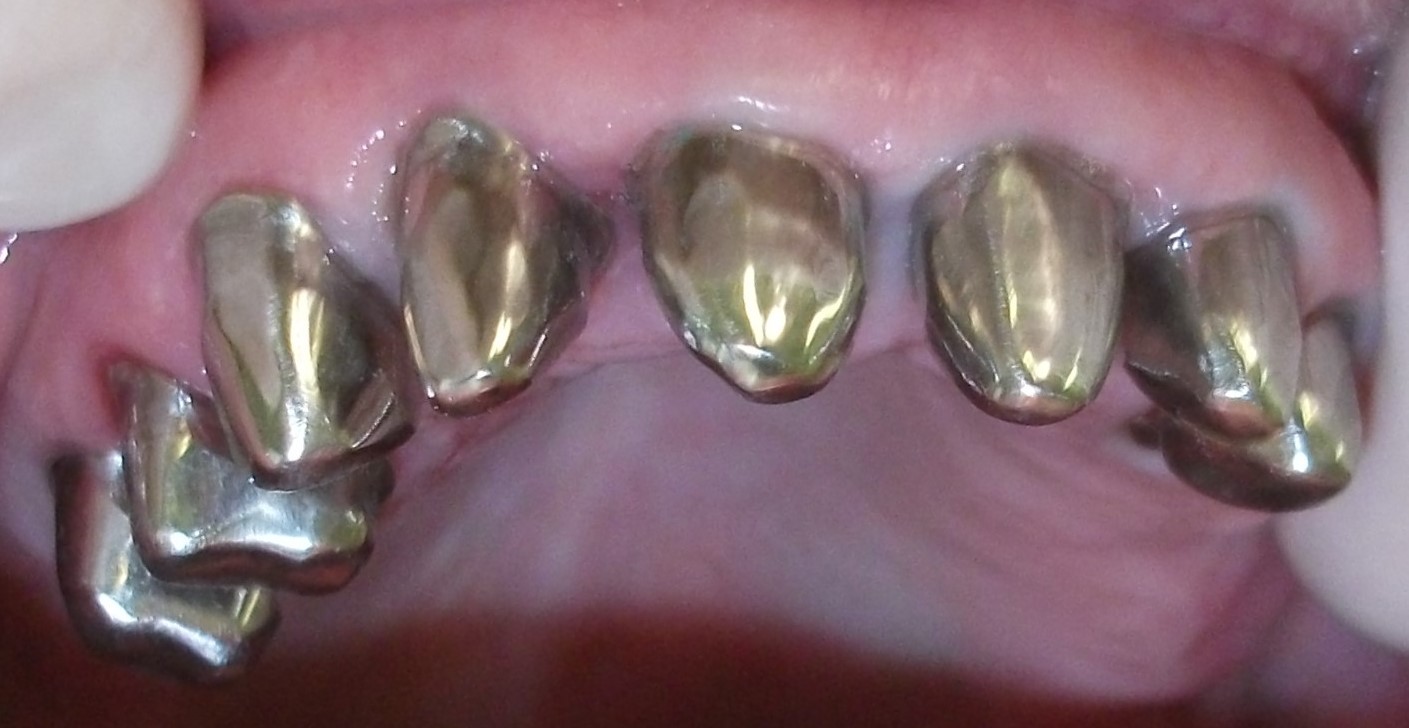 Fixed telescopic crowns (primary)
Fixed telescopic crowns (primary)
The patient-removable section with its retainers and connectors (e.g. clasps, precision attachments, telescopic crowns, press-stud systems, magnets etc.) is anchored on the periodontally-borne, fixed section of the restoration usually consisting of single crowns or bridge abutments supported on natural teeth, implants or implant abutments.
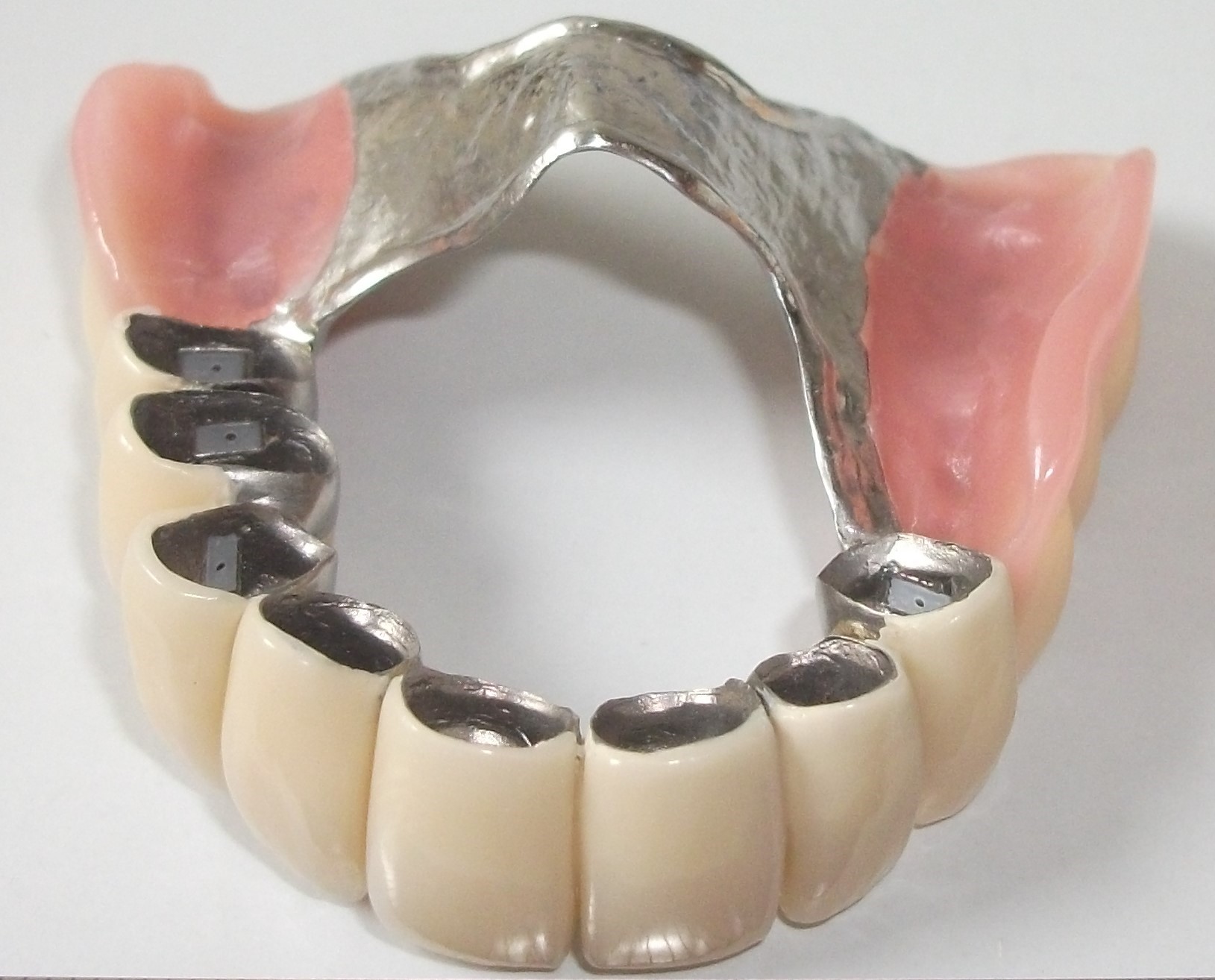 Removable partial denture (secondary section)
Removable partial denture (secondary section)
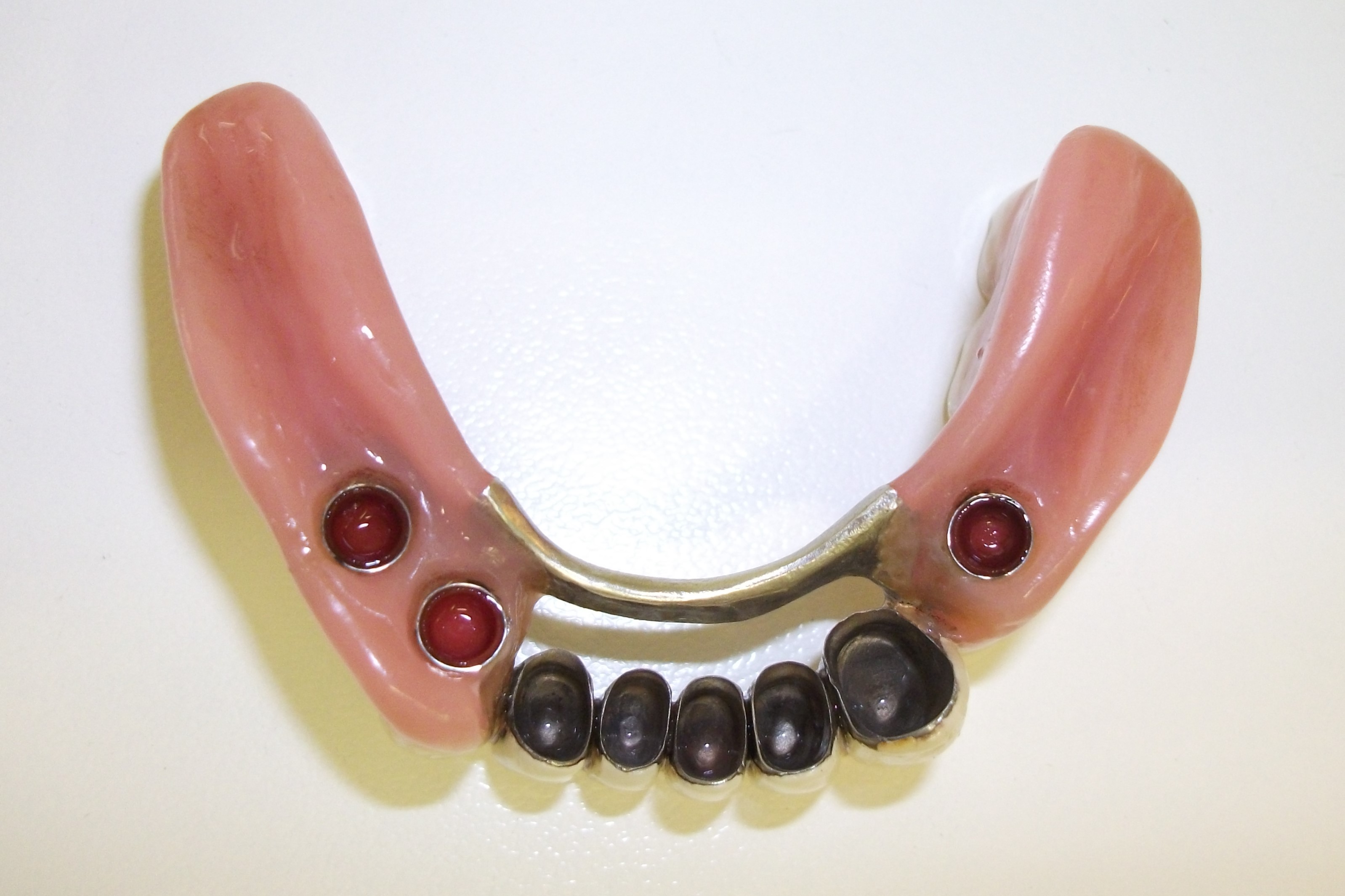 Removable lower partial denture
Removable lower partial denture
A removable bridge (usually "telescopic" and borne on telescopic crowns) replaces teeth with bridge units and almost never requires mucosal coverage.
Other types of fixed/removable prostheses always include sections which are supported by and exert pressure on the mucosa. A coverdenture fully covers all connectors and includes teeth corresponding to those of a full denture. That section of a fixed/removable prosthesis covering the hard upper palate is referred to as the palate and sections on edentulous areas of alveolar ridge are called saddles. In fixed/removable prostheses with multiple saddles they are often connected via a metal base – in the maxilla using a major connector (transverse) and via a lingual bar in the lower. Fixed/removable prostheses may also be totally metal-free. Missing teeth are usually replaced with prefabricated acrylic denture teeth and less frequently with prefabricated porcelain teeth.
When fabricating fixed/removable prostheses, special impression material and techniques are employed in an attempt to ensure that the denture base rests uniformly on the jaw. Exceeding the resilience of the mucosa or repeated "scrubbing" movements of the fixed/removable prosthesis may quickly result in pressure spots. After months or years, the bony denture base undergoes varying degrees of physiological and pressure-induced atrophy. The denture base can be relined to restore congruency.
Unlike purely fixed prosthetic restorations, fixed/removable prostheses can be cleaned and repaired extraorally. In addition, examining the residual dentition and maintaining its hygiene is easier. In case of loss of load-bearing abutments, fixed/removable restorations can often be extended without needing remaking.
Placing implants to increase the number of abutments supporting fixed/removable prostheses results in firmer, more stable retention and relieves the loading on the residual natural dentition.
Fixed/removable prostheses replacing not only missing teeth, but also other anatomical structures are referred to as maxillofacial appliances.
Tooth/implant-borne bridges are normally not considered to be fixed/removable restorations but rather purely fixed prostheses (possibly operator-removable) supported on natural teeth and implants.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| Knoop hardness test | Knoop-Härtetest |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

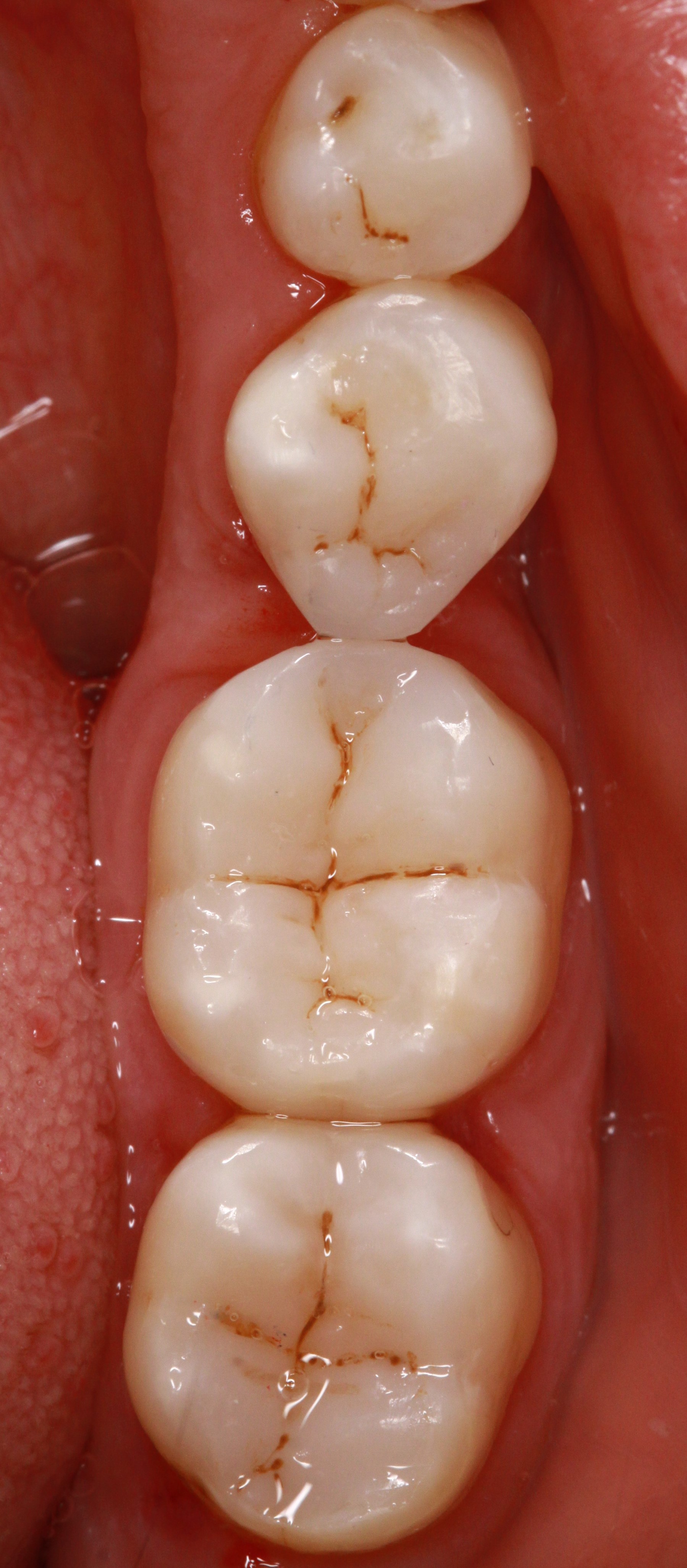
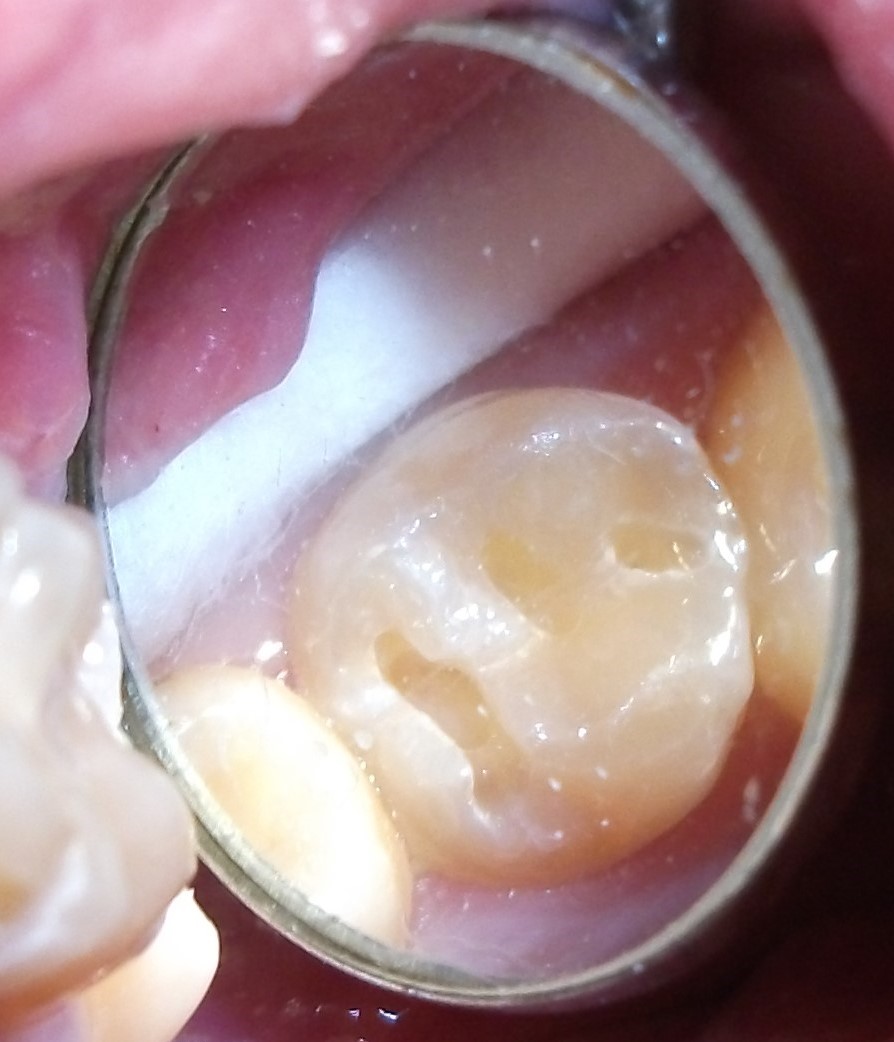 Minimally-invasive preparation and
Minimally-invasive preparation and 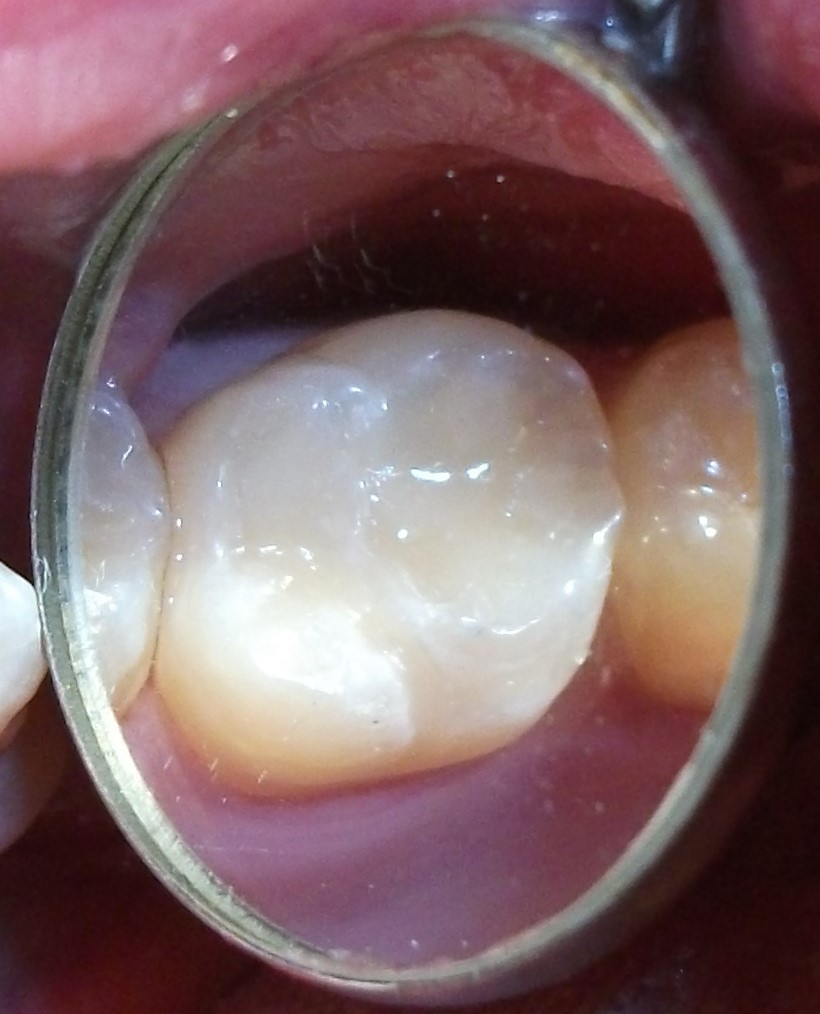 indiscernible composite restoration
indiscernible composite restoration