Sandblasters in dental technology
Sandblasters in dental technology
Frameworks are processed in the abrasive technique using appropriate sandblasters.
Handpieces are used in microblasters for manual blasting of individual frameworks. Recycling sandblasters are also available with integrated (adjustable) nozzles, which can also be used for simultaneously sandblasting several similar frameworks (e.g. CoCr castings) automatically in a slowly rotating blasting basket. Combination sandblasters incorporate the two functions.
Sandblasters are equipped with reservoirs (abrasive tanks) for one or more different abrasives (different grit sizes). Modern units often have a modular design and can simply be extended with other abrasive tanks as required for additional applications. Color-coding is used to facilitate identification and assignment of abrasives, handpieces/nozzles and system controls.
 A sandblaster
A sandblaster
The abrasive is directed onto the surface to be sandblasted using compressed air (preferably filtered, free from oil and water) as a jet through a fine nozzle, made from a highly resistant material (e.g. boron carbide). Accurate focusing of the jet increases the sandblasting precision and at the same time reduces the material consumption. The blasting chamber forms a self-contained work area. Used abrasive is trapped by filter systems and extractors, preventing indoor air contamination. Separators remove contaminants from the abrasive.
Viewing glass (the service-life is increased by using optional mesh guards), lighting and additional magnifying systems ensure a good view. Gloves (cuffs), which are permanently fixed in the unit housing, enable manipulation of the frameworks. Sandblasting is often activated using a foot-switch in order to keep the hands free.
Precise coordination of sandblasting pressure, grit size of the abrasive and distance and angle of the nozzle to the framework to be sandblasted are crucial in ensuring optimum sandblasting in the least possible and therefore more cost-effective time.
Modern sandblasters are suitable for universal use in all areas of application, e.g. the removal of residual investment and metal oxides, roughening to create retentive surfaces, high-luster or matt sandblasting, compacting metal surfaces as well as special applications such as cold silanization for coating surfaces in the RocatecTM system.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| translucent | transluzent |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

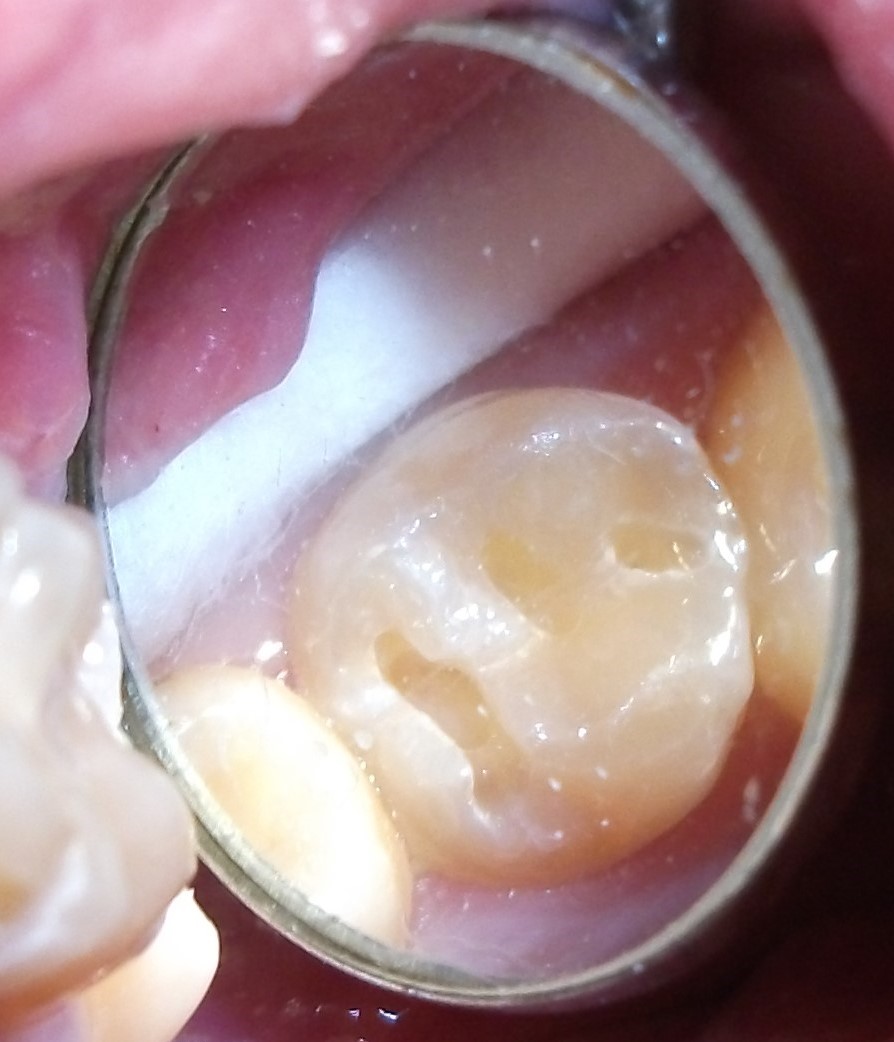 Minimally-invasive preparation and
Minimally-invasive preparation and 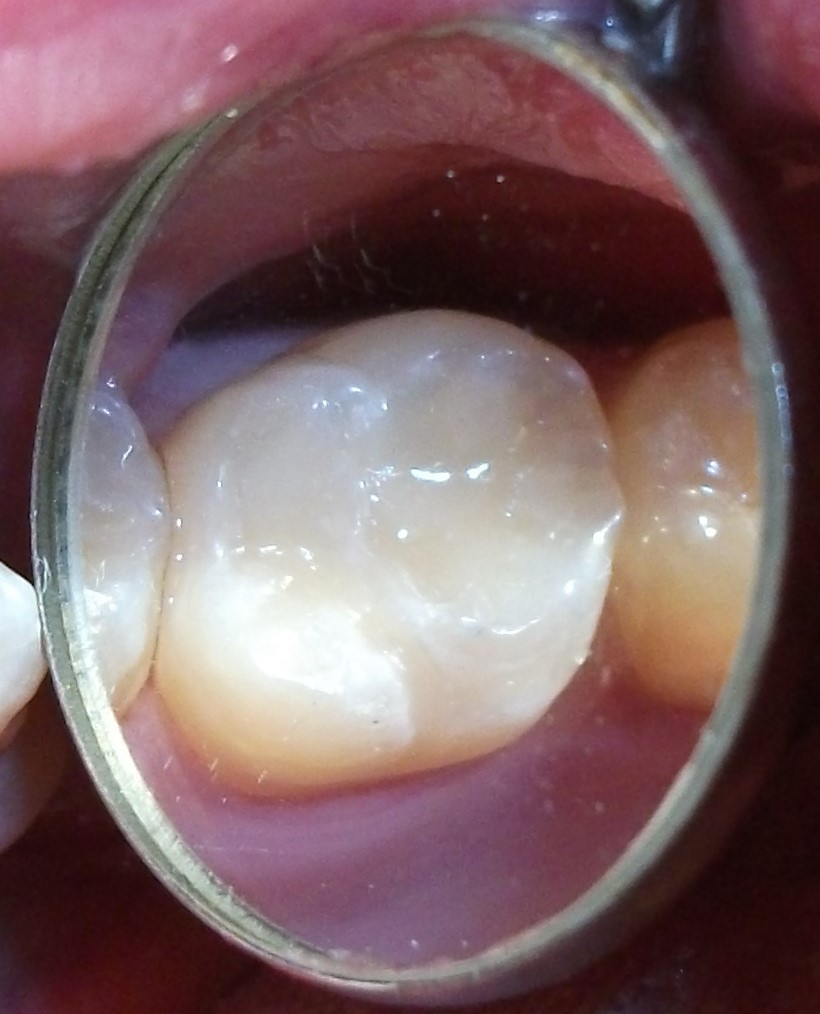 indiscernible composite restoration
indiscernible composite restoration