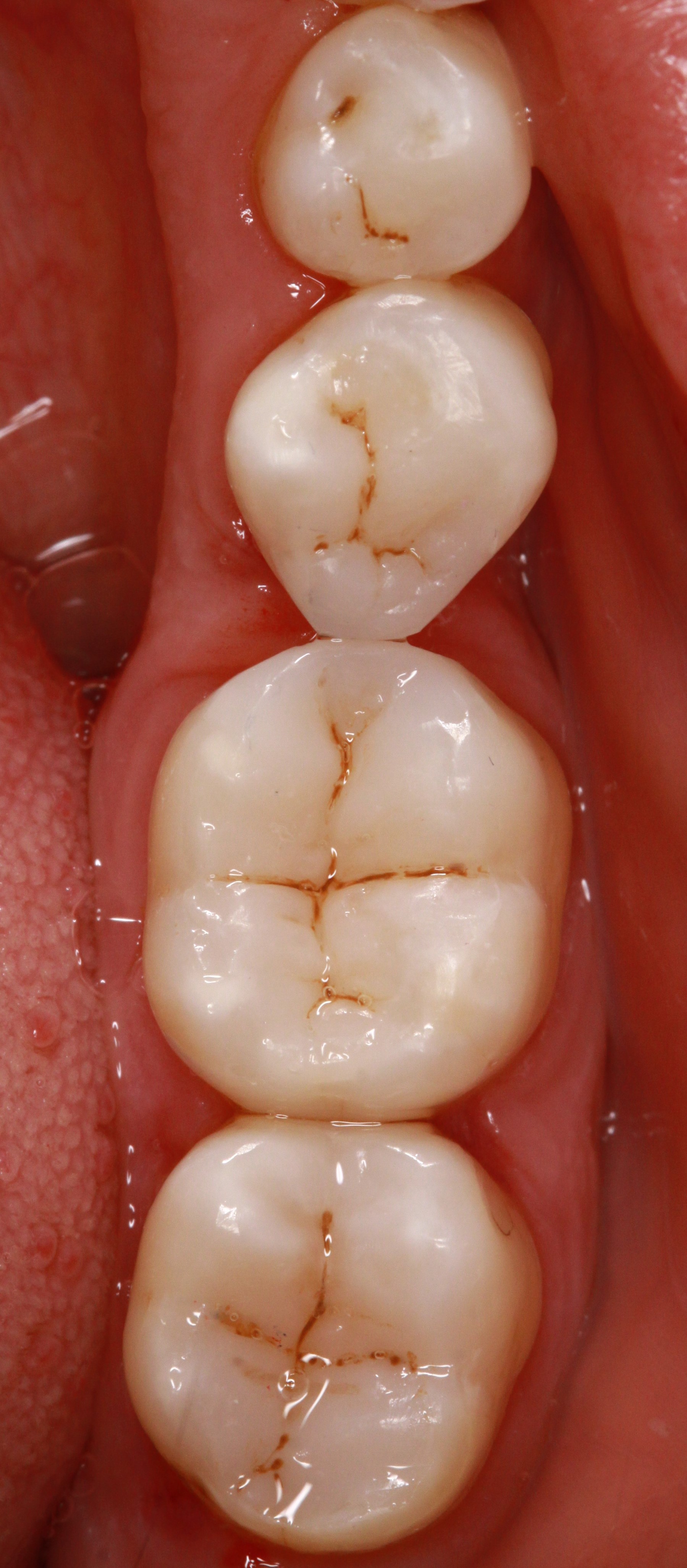
Glass-fibre ribbon
Glass-fibre ribbon (Splinting of teeth/reinforcing restorations)
A glass-fibre ribbon consists of glass drawn to very thin strands (diameter 10 µm to 20 µm). The resulting glass-fibres (“long fibres” >10 mm) can simply be twisted together (cords, mats) in the same direction lying next to each other or linked as with textiles to woven fabrics or meshes to increase significantly the dimensional stability and resistance to forces from different directions.
A composite material is created by embedding the glass-fibres in a different material (matrix). Though loose glass-fibres were first used in dentistry sporadically for reinforcing in the 1970s, the use of glass-fibre ribbons has become established since the 1990s.
Glass-fibres have a decisive advantage compared with other technically used fibres (e.g. carbon fibres), as they are transparent and aesthetically inconspicuous. The glass-fibre surfaces are silanized to improve the bond with the resin matrix. They are then impregnated (wetted) with a bonder/dental adhesive. The prefabricated ribbons in standard use today in the dental sector are divided into non-preimpregnated and preimpregnated (so-called prepregs).
Glass-fibre ribbons are used in different disciplines in dentistry with or without prepreparation of the tooth structure, e.g. in:
- Orthodontics: as a space maintainer for keeping tooth gaps open or as a retainer following completion of treatment
- Traumatology: for the fixation of teeth mobile due to trauma or that have been re-implanted (alternative to and/or in addition to metal splints)
- Implantology: for use during the healing period (long-term temporary restoration)
- Periodontology: as a periodontal splint
- Prosthetics: for temporary bridges that conserve the tooth tissue (e.g. also in the form of temporary restorations using natural teeth in which the natural tooth is used as a bridge unit) and minimally invasive permanent restorations, (e.g. with unilaterally fixed composite bridges in the case of inadequate bone availability in the anterior region.)
The glass-fibre ribbons must be handled with great care using metal instruments to avoid contamination of the bond surface with subsequent failure of the adhesive. Protected storage prevents drying out, material ageing or premature polymerisation. Application from a light-protected bottle greatly facilitates dispensing and significantly increases the shelf-life.
Many dental materials exhibit high compressive strength. Glass-fibres mainly improve the tensile strength and are, therefore, most effective when placed in tensile zones. Mechanical properties of the bond are influenced by various factors: the proportion of fibre and matrix should be in the region of 50% each to utilise the advantages of the glass-fibre and avoid cohesive fractures within excessively thick composite regions. Pre-impregnated ribbons are already manufactured in this manner. They should be placed close to the tooth (with splinting, collar-shaped in the interdental space) and fill the framework to be fabricated as completely as possible.
After a splint or restoration is finished, the glass-fibres should always be covered thinly but completely by composite (to prevent chipping and swelling due to water intake). Generally, flowable, low-filled composite materials (flowables) are applied using the brush technique for covering the fibres.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| micromovement | Mikrobewegung |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

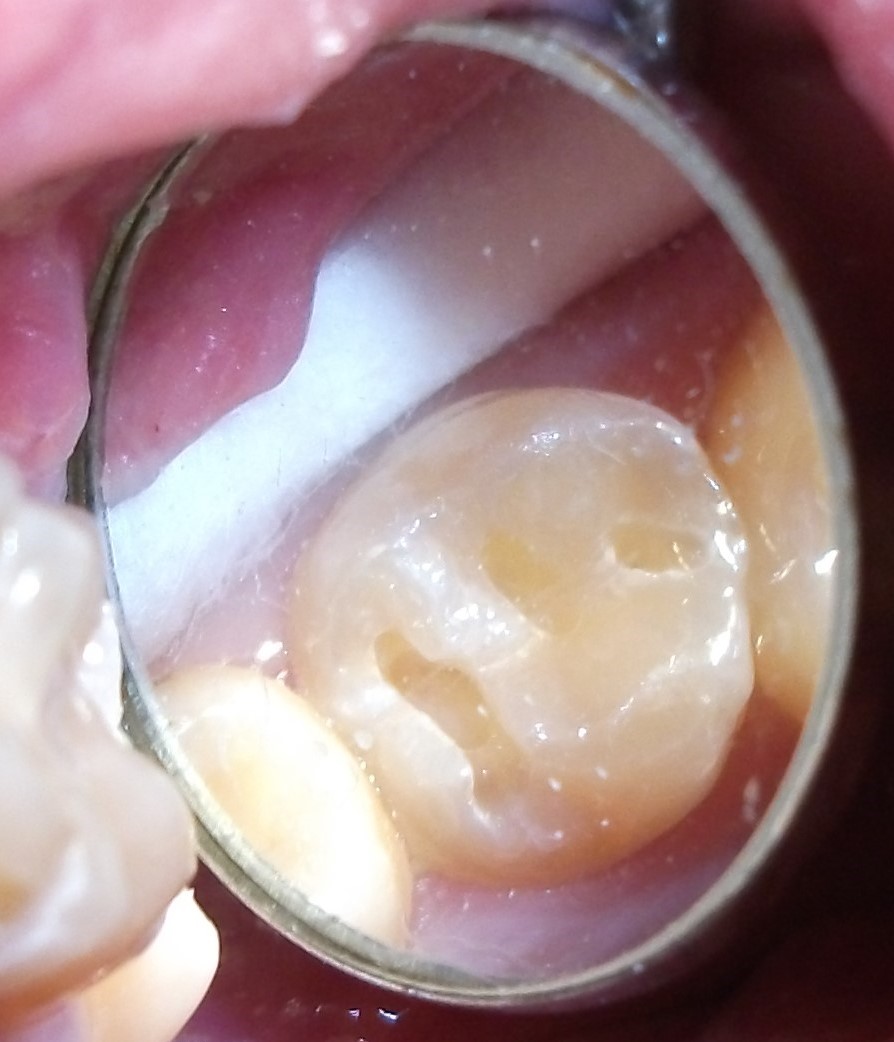 Minimally-invasive preparation and
Minimally-invasive preparation and 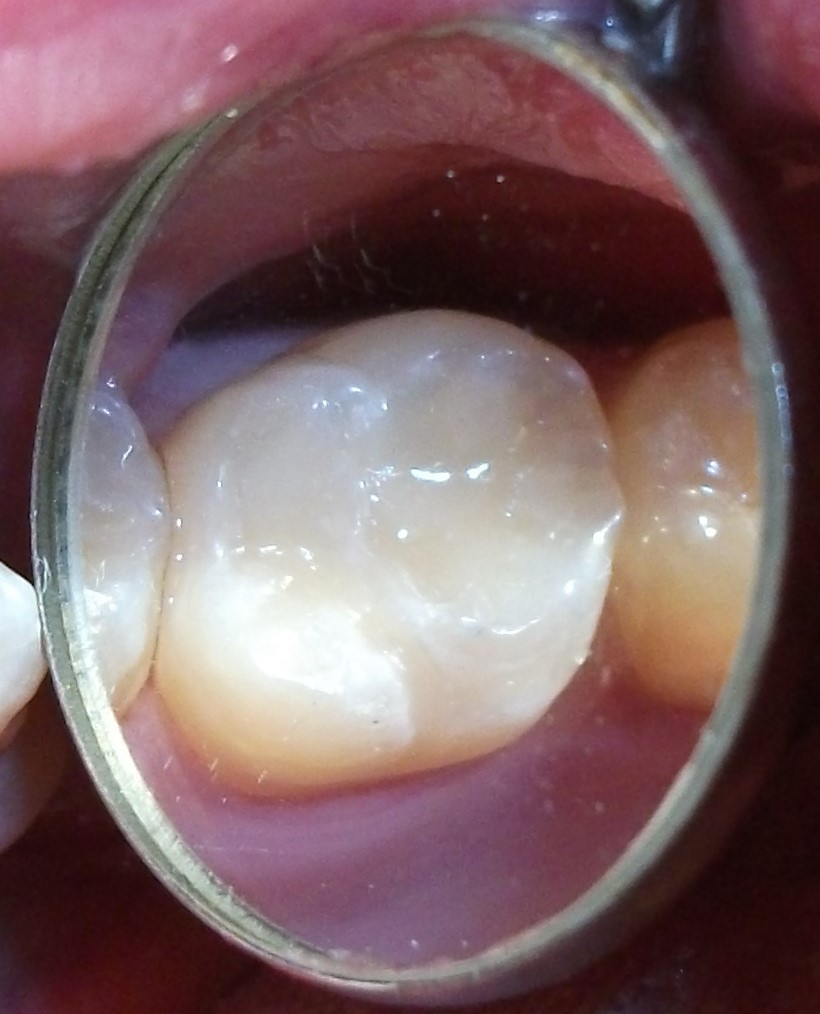 indiscernible composite restoration
indiscernible composite restoration