Intraoral scanners
Intraoral scanners
An intraoral scanner is an electronic device for taking so-called digital scans (impressions) of intraoral structures by means of contactless scanning with light rays (visible light/laser) chairside and within seconds or minutes. These devices comprise (as of 2016) a wired handpiece, for intraoral use by the dentist, connected to a computer system with monitor. A combination of a special camera unit in a known three-dimensional position to a light source uses triangulation to calculate the three-dimensional arrangement of the light reflecting surface points of the scanned structures with an accuracy of 20 µm. Each measuring field is usually only about two square centimetres in size but many images (20 to 60 mostly colour video/series images per second) can be taken and merged in quick succession.
To achieve an accurate intraoral scan, (as with every conventional impression) undercuts (possibly non-detectable optically) must be avoided, other obscured (by retraction pastes and cords) areas such as subgingival regions exposed in advance and bleeding staunched. To date, intraoral scanners cannot capture mucosal resilience (important for designing denture bases).
Some systems require additional preparation by coating the imaging area with a thin layer of powder. Implant platforms and their connector geometry are scanned indirectly by placing “scanbodies” i.e., standardised components of known dimensions and clearly aligned three-dimensionally via standardised recesses, on their top surfaces.
When preparing teeth, in real-time parameters such as amount of reduction in tooth structure, distance from opposing dentition, path of insertion and parallelisation of abutment teeth, surface morphology or contours of the preparation margin may be blown-up as required for evaluation and adjustment if necessary. In addition to teeth and/or implants for replacement or treatment, adjacent and opposing teeth as well as the bite may be scanned.
Full digital scans of a jaw may be captured in one procedure or merged one-by-one from overlapping partial images. Specific regions are easily cut out, re-scanned and blended in as often as required.
The scan data are converted into firmware data formats (such as STL), usually exportable into third-party systems, using specific software and calculated to create a virtual, three-dimensional model which can be viewed on the monitor.
The data can be supplemented and further processed with additional CAD and CAM programmes e.g., for placing virtual implants, planning and fabricating restorations, abutments, drilling templates, bite raisers or producing real models. When used with manufacturing equipment (such as milling machines), restorations such as veneers, inlays, crowns or short-span bridgework can be fabricated in a single appointment.
Intraoral scanners are an increasingly relevant alternative to taking conventional impressions with elastomeric impression materials (PVS, polyether, etc.). Less material is required, breathing is not obstructed and gagging as well as risk of aspiration no longer occur. This very first important step already provides an entry-point to digital workflow, without having to “divert” via error-prone “real” impressions and models followed by scanning them with extraoral equipment (“lab scanners”).
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| translucent | transluzent |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

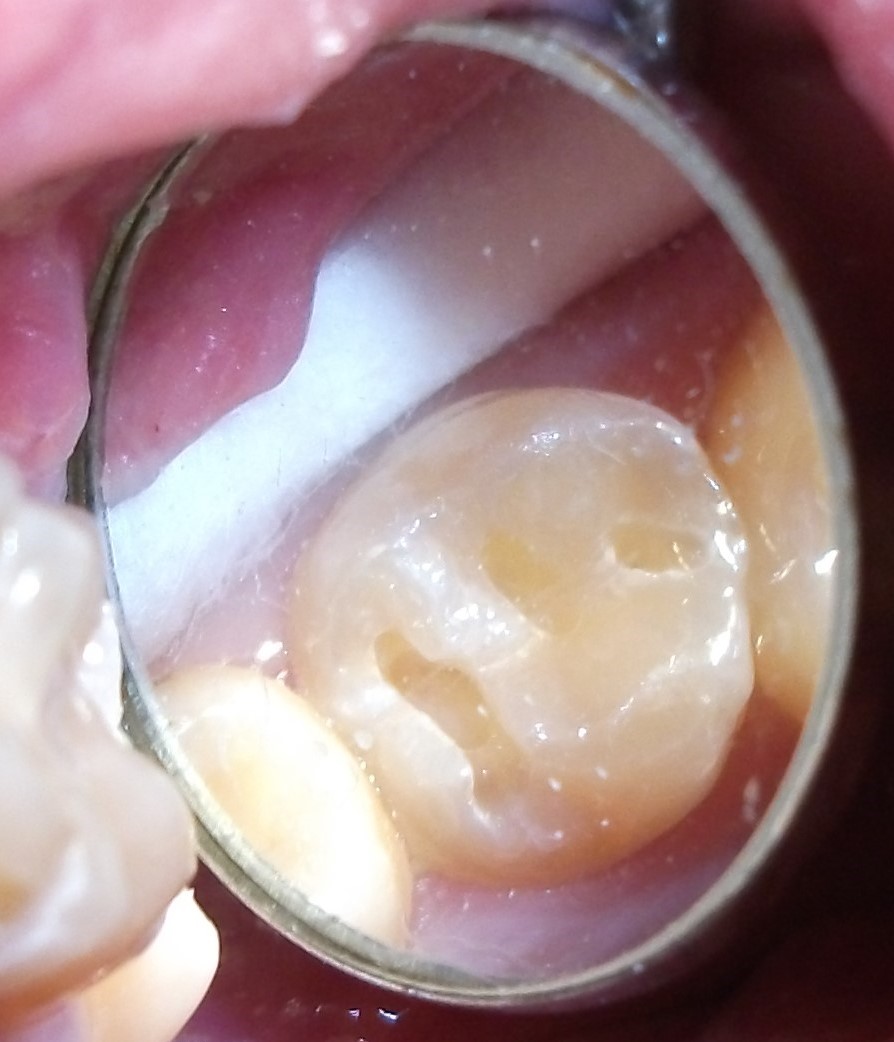 Minimally-invasive preparation and
Minimally-invasive preparation and 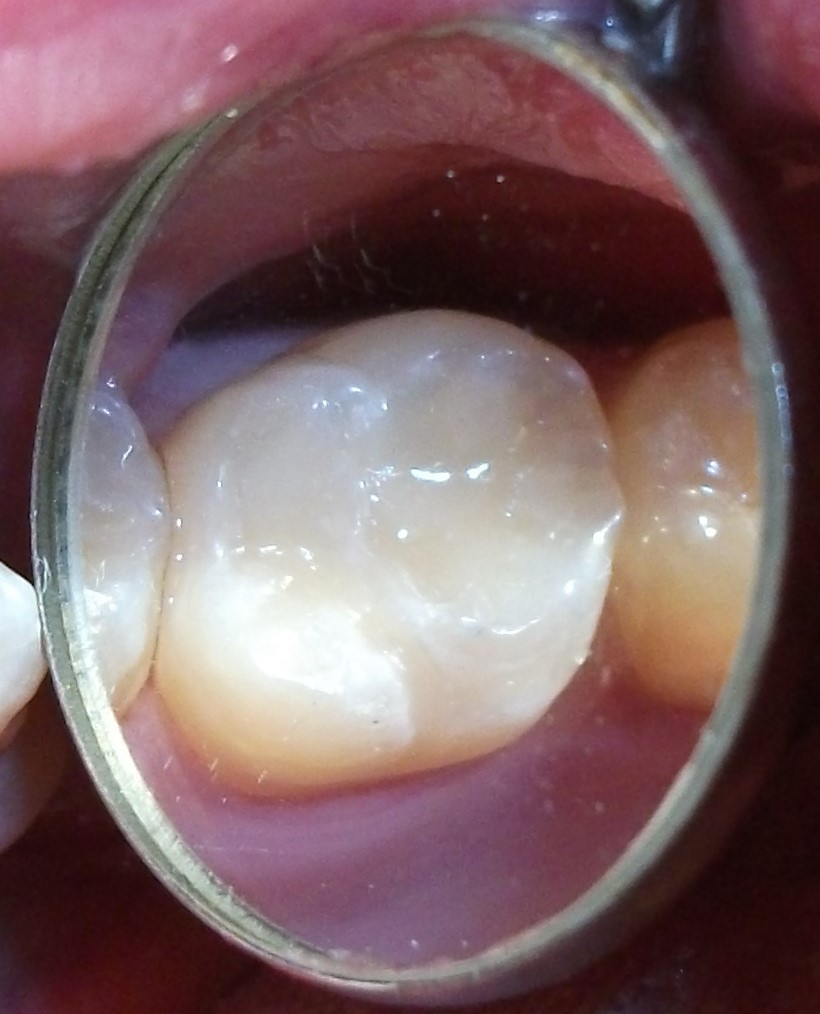 indiscernible composite restoration
indiscernible composite restoration