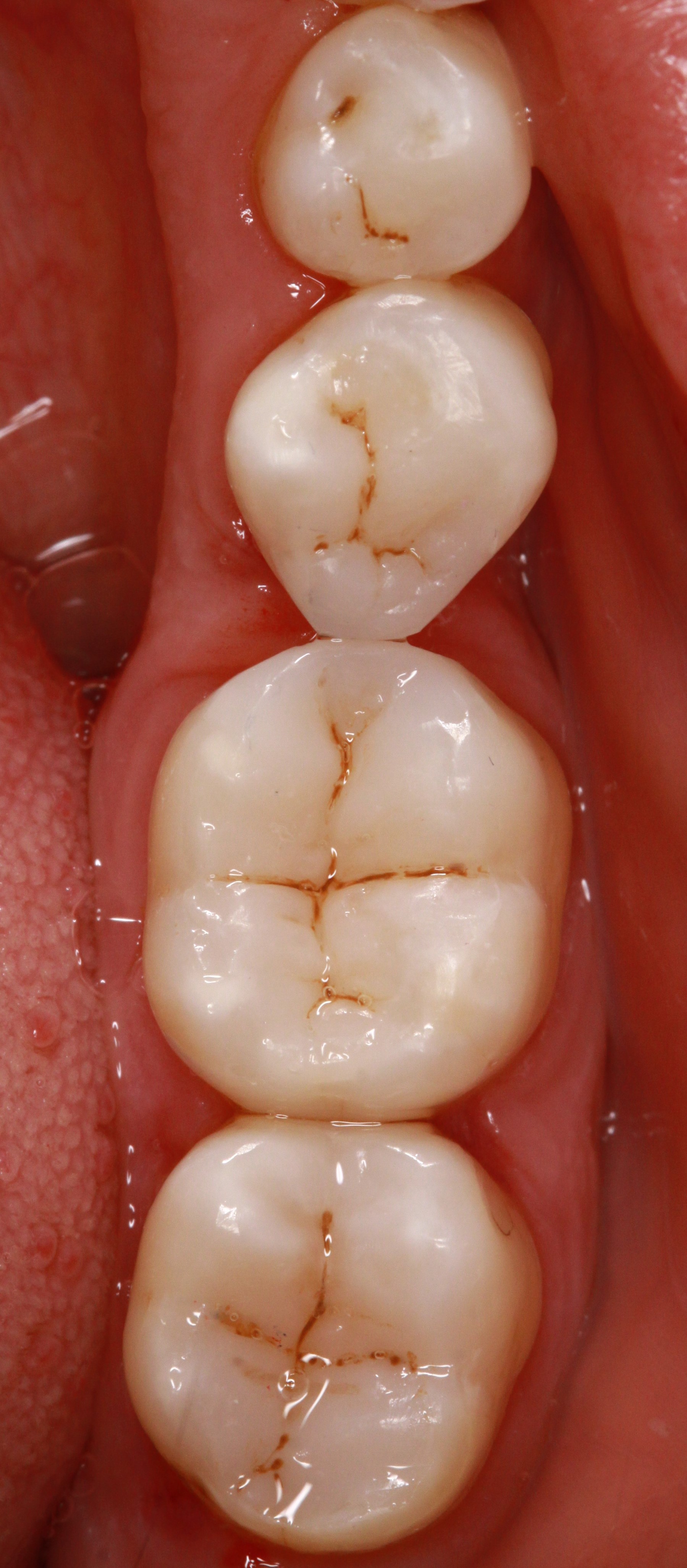
CMD
CMD (craniomandibular dysfunction) is a collective term for different types of disorders of the normal function of the masticatory organ (also called "masticatory apparatus", comprising teeth, jaws, tongue, temporomandibular joints, masticatory musculature, neural circuits involved and adjacent anatomical structures) with multiple symptoms. Alternative terms are craniovertebral dysfunction (CVD), myoarthropathy, stomatognathic dysfunction, temporomandibular dysfunction (TMD) etc.
The symptoms of CMD can be roughly divided into the areas of joint problems (arthropathy), displacement of the disc (discopathy), myofacial pain (myopathy) and other physical and psychological symptoms. In particular in the temporomandibular joint it can lead to pain, cracking or rubbing noises, restriction of the mouth opening or even to lockjaw. There may be lateral deflection, deviation from the straight, vertical mouth opening. Increased mobility of the mandible is also possible; the mandible can also dislocate (lockjaw, luxation), e.g. with a wide yawn. Frequently tension and pain may occur in the regions of the masticatory musculature, head, face and neck. In rare cases earache, ringing in the ears (tinnitus), dry mouth or taste disorders can also occur.
In addition to a general dental examination and diagnosis, first an orientating test (rapid test) is required in cases with indications for CMD followed by comprehensive diagnosis of the masticatory system (functional analysis, functional diagnostics) for detection and more precise determination of CMD. This includes manual examination of temporomandibular joints and musculature (manual functional analysis), with special measuring devices (instrumental functional analysis) and often also special X-rays (temporomandibular joint X-ray) as well as standardised questionnaires for collecting specific patient case histories. Findings are recorded and evaluated in a standardised form (functional status).
Apart from general illnesses (rheumatics, arthritis, muscle and nerve diseases), possible causes of CMD are congenital and acquired tooth malalignment (tipping, rotation, extension), intercuspation and occlusal relationship disorders ("occlusopathy", cross-bite, edge-to-edge bite, deep overbite, open bite), diastemas, incorrect vertical relationship of dentures, bridges, crowns or fillings, misalignment of the locomotor system, accidents, overloading and overstretching (power sports, intensive chewing of gum, long-term tooth treatments, operations under general anaesthetic, parafunctions (habits) such as biting nails/pencils and bruxism (clenching, grinding) and also stress and mental/psychological strains and disorders (psychosis, depression, anxiety disorders). There is seldom only one single cause; mainly several factors are collectively involved in the development of CMD (multifactorial aetiology).
Many dysfunctions are low grade and harmless. Serious dysfunctions can also be pain-free (referred to as "compensated CMD") or accompanied by passages of pain to frequent and/or long-lasting pain. Long-term dysfunction can result in damage to parts of the masticatory apparatus, in particular to teeth (heavy attrition), periodontium (periodontitides) and temporomandibular joints (attrition, habitual luxation) and also to persistent neuropathies ("trigeminal neuralgia"). Clearly identifiable, disturbing or painful CMD should therefore be treated.
Mutual interaction between CMD in the cranial region, changes in posture and other further-removed sections of the locomotive system, (musculoskeletal system), e.g. head, neck, shoulders, vertebral column, hips, knee and feet) as well as psychological factors often render interdisciplinary collaboration therapeutically practical, for instance between the dentist, orthopaedist, physiotherapist, psychotherapist etc.
Initially, easily reversible and/or less invasive (minimally invasive) treatment options are selected, such as short-term pain relief (using analgesics, cold or warm application), prevention and self-help (light food, movement and relaxation exercises), physical and physiotherapy, psychosomatic medicine and also removable splints. Different types of laboratory-fabricated splints are regularly used during treatment of CMD. The objectives of splint therapy include: reversing and re-orientation of the masticatory system, relaxation of the musculature; changing the position of the condylar head (retraction, reposition, distraction; protection of teeth and restorations against attrition, cracks, breaking off and protection of the periodontium against overloading.
Irreversible (invasive) treatment approaches (e.g. heavy systematic grinding-in, restoration, orthodontics, operations) are mainly reserved for serious courses of diseases.
CMD and other areas of dentistry are closely interrelated: CMD should be excluded or treated (to ensure success) before undertaking extensive (conservative or prosthetic) restorations, if necessary these will also be fitted to safeguard a new pain-free "therapeutic" occlusal relationship acquired during CMD treatment. Orthodontic treatment is intended to avoid favourable conditions for CMD, though it can also be used for its treatment. Conversely, CMD therapies can display orthodontic effects.
All aspects of CMD have been the subject of intensive technical dispute for decades between sometimes mutually exclusive approaches. In addition to terminology, aetiology, diagnostics, manifestation and meaning of CMD, all treatment approaches (whose evidence-base encounters systematic difficulties) are fundamentally called into question time and again.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| non-threaded | gewindelos |
Focus text of the month
Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic… Composites also composite (from the Latin componere = to compose) are tooth-coloured filling materials with plastic properties used in dental treatment. In lay terms they are often referred to as plastic fillings, also erroneously sometimes confused with ceramic fillings due to their tooth colour. After being placed in a cavity they cure chemically or by irradiating with light or a combination of the two (dual-curing). Nowadays, composites are also used as luting materials. The working time can be regulated with light-curing systems, which is a great advantage both when placing fillings and during adhesive luting of restorations. Dual-curing luting materials are paste/paste systems with chemical and photosensitive initiators, which enable adequate curing, even in areas in which light curing is not guaranteed or controllable. Composites were manufactured in 1962 by mixing dimethacrylate (epoxy resin and methacrylic acid) with silanized quartz powder (Bowen 1963). Due to their characteristics (aesthetics and advantages of the adhesive technique) composite restorations are now used instead of amalgam fillings.
The material consists of three constituents: the resin matrix (organic component), the fillers (inorganic component) and the composite phase. The resin matrix mainly consists of Bis-GMA (bisphenol-A-glycidyldimethacrylate). As Bis-GMA is highly viscous, it is mixed in a different composition with shorter-chain monomers such as, e.g. TEGDMA (triethylene glycol dimethacrylate). The lower the proportion of Bis-GMA and the higher the proportion of TEGDMA, the higher the polymerisation shrinkage (Gonçalves et al. 2008). The use of Bis-GMA with TEGDMA increases the tensile strength but reduces the flexural strength (Asmussen & Peutzfeldt 1998). Monomers can be released from the filling material. Longer light-curing results in a better conversion rate (linking of the individual monomers) and therefore to reduced monomer release (Sideriou & Achilias 2005) The fillers are made of quartz, ceramic and/ or silicon dioxide. An increase in the amount of filler materials results in decreases in polymerisation shrinkage, coefficient of linear expansion and water absorption. In contrast, with an increase in the filler proportion there is a general rise in the compressive and tensile strengths, modulus of elasticity and wear resistance (Kim et al. 2002). The filler content in a composite is also determined by the shape of the fillers.
Composite restorations Conclusion |

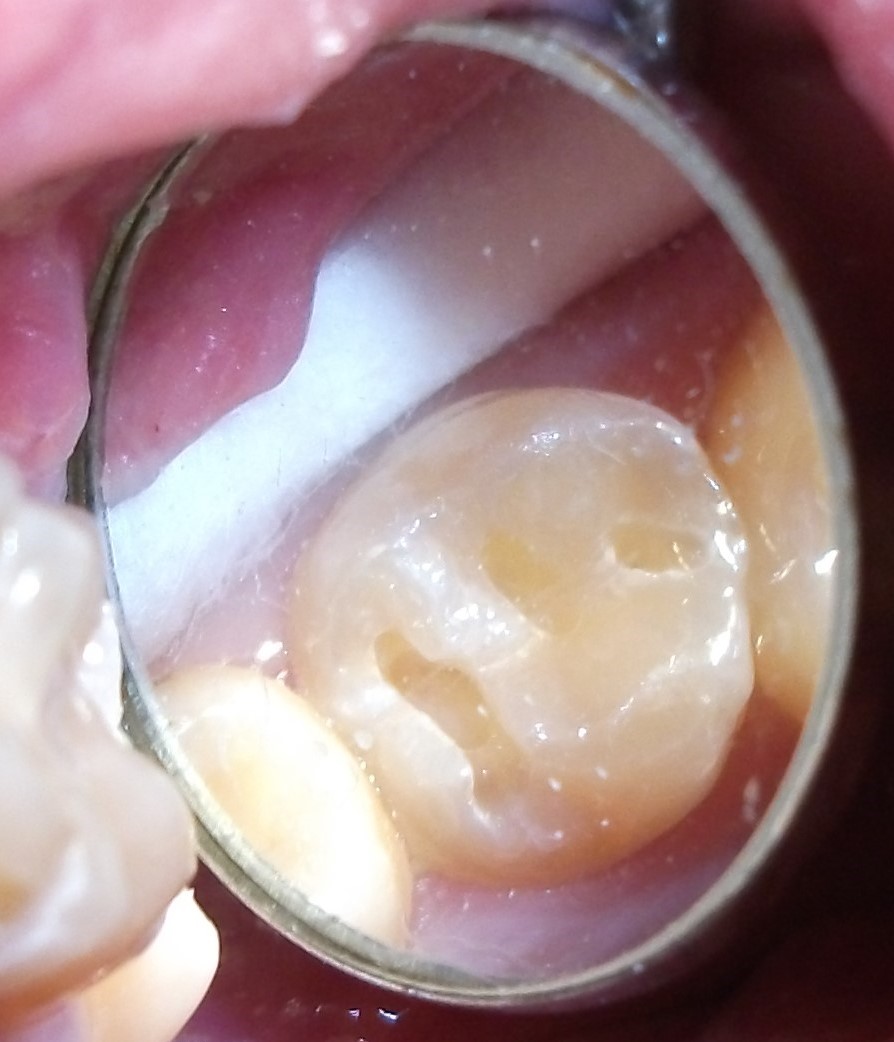 Minimally-invasive preparation and
Minimally-invasive preparation and 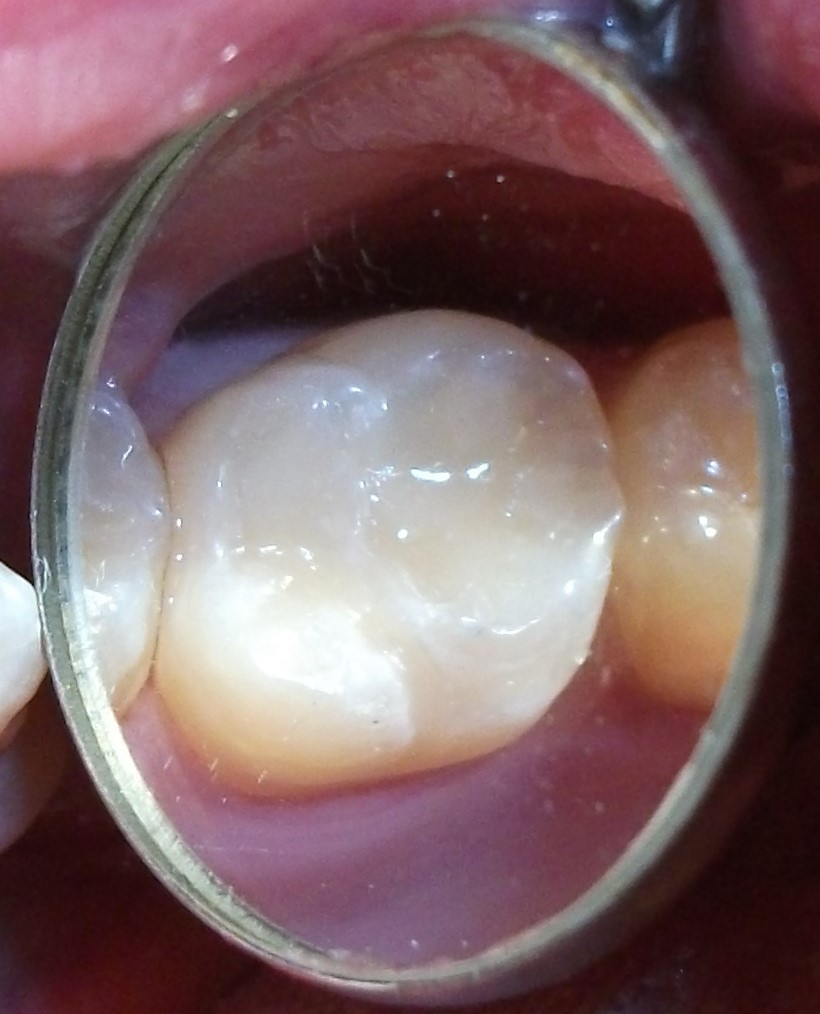 indiscernible composite restoration
indiscernible composite restoration