X-rays
X-rays
The invisible roentgen rays named after Wilhelm Conrad Röntgen (German physicist, 1st physics Nobel prize 1901 (initially referred to as "X-rays" in German, still called X-rays today in English]) are used for therapeutic, but mainly for diagnostic purposes in medicine, dentistry, structure and material testing.
The electromagnetic (ionising, i.e. uncharged molecules dispersed in ions and electrons) roentgen rays have shorter wavelengths than visible light. They penetrate body tissue and are biologically harmful, e.g. carcinogenic, (cancer-causing), mutagenic (gene-changing) and teratogenic (embryo-damaging). This is why the frequency (i.e. the number of X-ray images) and the respective single dose must be limited to the absolutely necessary in order to minimise radiation exposure. Areas that should not be irradiated must be shielded using suitable materials (mainly lead, e.g. in X-ray shields, radiography aprons, X-ray protective doors etc.).
Diffraction of X-rays allows conclusions to be made about the structure of molecules (DNA), crystals and materials. Emission of element-typical spectra of X-rays after irradiation with electrons or X-rays (X-ray fluorescence) enables analysis of the chemical elements contained in the substances.
Orthopaedic pain levels ("X-ray inflammation irradiation") and tumour cells, which are sensitive to radiation, can be combated using X-rays. The (e.g. intraoperative) X-raying of body structures (using radiographic image intensifiers) is used for analysis of processes and optimisation (e.g. reposition of fractures).
Occasions for using diagnostic X-rays can be acute complaints, traumata or disease status, but also exclusion and early diagnosis of damage (bitewing X-ray for early detection of caries) as well as planning and follow-up of dental treatment measures (surgery, endodontology, implantology, orthodontics, prosthetics).
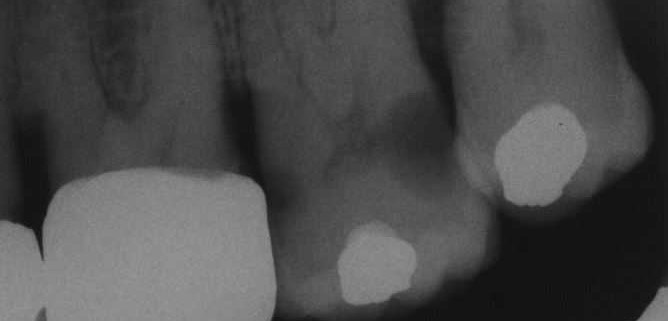 Extensive carious cavity in tooth 27
Extensive carious cavity in tooth 27
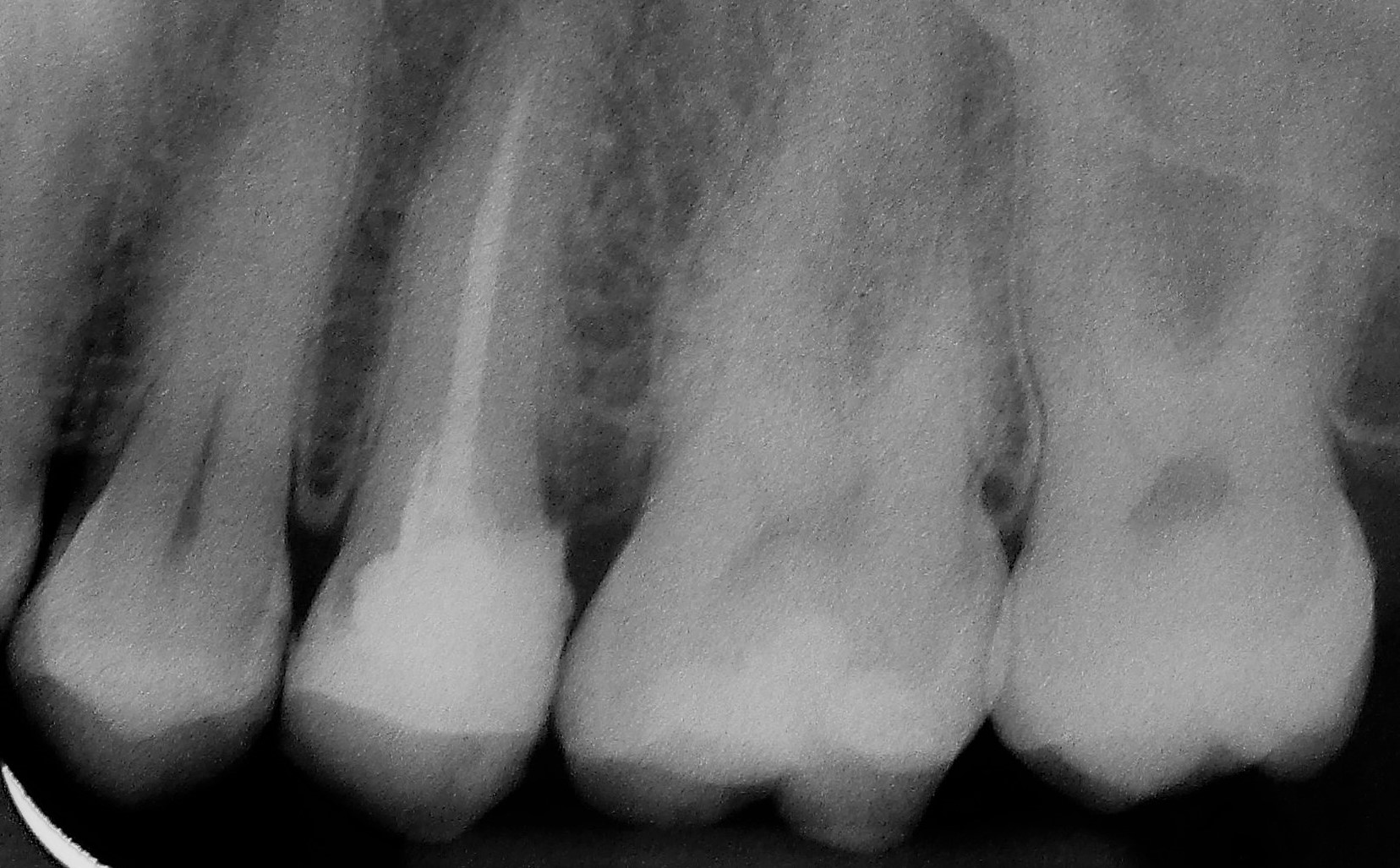 X-ray image
X-ray image
In dentistry intraoral X-ray tubes (X-ray sources) are rarely used, though extraoral X-ray tubes are mainly used to irradiate analogue, light-sensitive X-ray films (chemical development and fixation in the darkroom), X-ray imaging plates (stimulation of fluorescent substance, scanning using lasers) or digital X-ray sensors (CCD or CMOS semiconductor devices). The X-ray voltage of "conventionally" used X-rays is 60 to 70 kilovolts. Two-dimensional images are created using static systems (dental film, lateral cephalometric radiograph, temporomandibular images) and orthopantomograms and three-dimensional images (CT = computer tomography, CBCT = cone-beam computed tomography) are created using rotary systems. The images are viewed on X-ray viewers (analogue) or (if necessary, combined with image processing) on the computer monitor (digital).
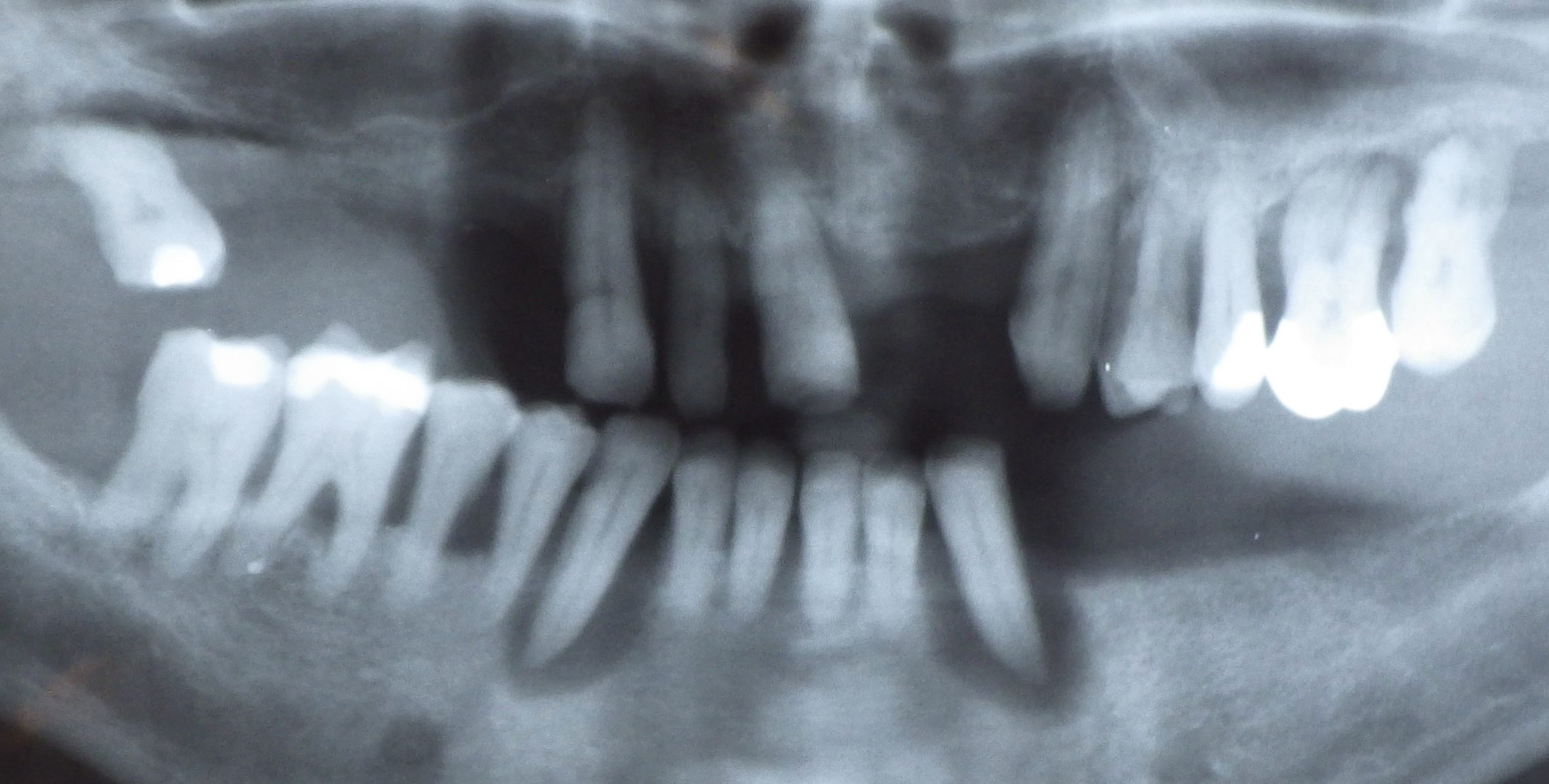 Panoramic X-ray, orthopantogram
Panoramic X-ray, orthopantogram
.jpg) Orthopantogram of an 8-year-old (deciduous dentition)
Orthopantogram of an 8-year-old (deciduous dentition)
Different body tissues contain varying amounts of chemical elements whose proton count in the atom nucleus differ and consequently their absorption of the X-rays, which shows as image contrast, e.g. between hard structure with a different calcium content (bone, dentine, dental enamel) and soft tissue. A greyscale image is created with a resolution of up to 20 line pairs per millimetre or 25 µm. The usual negative representation leads to correspondingly "reverse" terminology, lighter areas are defined as shadowing and darker areas as brightening.
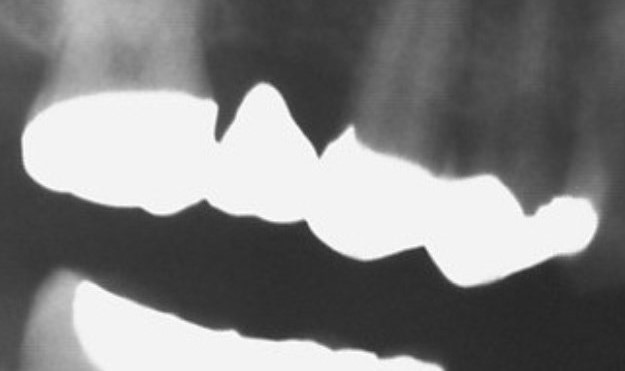 Bridgework spanning teeth 15 - 17
Bridgework spanning teeth 15 - 17
Metal foreign bodies (amalgam, cast restorations) and ceramics placed in the oral cavity normally have a high degree of radiopacity and appear white or light grey. Filling materials (temporary sealers, composite and gutta percha) medication (calcium hydroxide paste) or acrylics and denture teeth for X-ray templates can be made radiopaque using positive X-ray contrast materials.
Want to give it a try ...
... or need professional advice?
Get in touch with us or click Contact.
Word of the day
| English | German |
|---|---|
| anamnesis form | Anamnesebogen |
Focus text of the month
Wax build-up technique Wax build-up technique The various anatomical structures (such as cusp tips and slopes as well as marginal ridges) are usually built up one after another by adding small portions of wax (often using differently coloured waxes for didactic purposes). The firm, special waxes first have to be melted at room temperature. This can be carried out by warming small portions on differently shaped working tips of hand instruments in an open flame (such as a gas burner) or using electrically heated instruments which provide for more accurate temperature control and avoid contamination (e.g. electric wax-knife, induction heaters, wax dipping units). The wax is applied drop-by-drop to ensure that the warmer molten wax added last fuses seamlessly with the firm, cooler material. After hardening, the wax pattern can be reduced by sculpting, milling guidance surfaces or drilling to add retainers. Modern procedures include flexible, occlusal preforms for adding contours to soft wax. In addition, wax preforms, such as for occlusal surfaces or bridge pontics, are available in various shapes and sizes. Recently, irreversible, light-curing materials have been introduced for use instead of reversible thermoplastic waxes.
To ensure that the wax pattern can be released without being damaged, model surfaces, opposing dentition and preparations must be hardened/sealed with special lacquer (applied by spraying, brushing or dipping). These waxes are mostly relatively rigid/elastic after cooling.
When employing the lost wax technique, prefabricated wax sprues, bars and reservoirs are attached to the patterns. Once the pattern has been released and its sprues waxed onto the crucible former, it is invested in a casting ring with refractory investment material. The wax can then be burnt out residue-free and casting completed. Unlike standard wax build-up techniques, a diagnostic wax-up is not intended for fabricating an indirect restoration, but rather for simulating the appearance and/or external contouring for producing orientation templates. |

 Wax preforms
Wax preforms Attaching wax sprues to a removable framework supported on double crowns using a hand instrument
Attaching wax sprues to a removable framework supported on double crowns using a hand instrument